If you read the first part of our iron education series on iron homeostasis, you already know the story: conventional iron supplements often fail because they ignore the body's regulatory machinery. Hepcidin, the hormone that controls how much iron your body absorbs and circulates, gets thrown off by inflammation, and when that happens, adding more iron doesn't fix the problem.

Iron and immunity aren't separate systems -- they share the same signals. Lactoferrin sits at that intersection, and effera® delivers it in the human-identical form your body actually recognizes.
But there's a second half to that story.
Iron and the Immune System: An Undervalued Piece of the Iron Puzzle
The relationship between iron and your immune system doesn't just run one direction. Yes, chronic inflammation disrupts your iron status. But the reverse is also true: when your iron regulation breaks down, your immune function takes a hit too. These two systems are intertwined, sharing the same signaling molecules, the same feedback loops, and many of the same protein players.
In this article, we break down the iron-immunity connection, explain lactoferrin's dual role as an immune modulator and iron regulator, review key human studies on inflammatory markers, and share practical takeaways for supplementation with effera®, human-bioidentical lactoferrin from Helaina.
Sign up below for updates on Helaina and effera® so you'll catch future installments as we continue building this series:
Subscribe to PricePlow's Newsletter and Alerts on These Topics
If you missed the first article in this series, read Iron Homeostasis and effera® Human Lactoferrin: Beyond the "More Iron" Myth before continuing. It lays the foundation for what we cover here.
Iron and Immunity: Two Systems, One Shared Language
Your immune system and your iron regulatory system communicate through the same chemical messengers. The most important one for this discussion is interleukin-6 (IL-6). Think of IL-6 as an alarm signal: a protein (called a cytokine) that your immune cells release when they detect a threat. As we covered in the first article, IL-6 directly tells your liver to produce more hepcidin, which then locks iron away from circulation. That's your body's way of starving bacteria and other pathogens that depend on iron to survive.[1]

More iron won't fix deficiency when inflammation blocks absorption. Lactoferrin supports iron homeostasis by reducing inflammation and restoring balance.
The problem is that this protective mechanism can become chronic. When inflammation persists due to poor diet, metabolic stress, ongoing illness, or heavy training loads, elevated IL-6 keeps hepcidin elevated too, and iron stays locked up even when your body genuinely needs it.
The road also runs the other direction. Iron-deficient immune cells are functionally impaired. Your white blood cells (the soldiers of your immune system) depend heavily on iron to divide, generate energy, and produce the reactive compounds they use to neutralize threats. When iron is chronically low, immune cell activity drops alongside it.[2]
The result is a self-reinforcing negative feedback loop. Chronic inflammation depletes functional iron. Iron deficiency weakens immune cells. Weakened immune cells can't resolve the underlying inflammation. Round and round it goes. One of the most important things in health is breaking negative feedback loops like this, and Helaina has just the tool.
Treating iron and immunity as separate problems misses this shared biology. Lactoferrin, the iron-binding protein found in human milk and released by your own immune cells, sits at the intersection of both systems, and that positioning is not coincidental.
Lactoferrin Is Part of Your Immune System
Here's something that surprises most people when they first learn it: lactoferrin isn't just something that binds iron, and it's not just found in milk. Your immune system produces it, too.
When your body detects an infection or injury, a type of white blood cell called a neutrophil (your immune system's first responders: cells that arrive at a threat site within minutes) releases stored lactoferrin directly at the site of the problem. The fact that your body stores lactoferrin in immune cells and deploys it during active immune responses makes clear that it's a built-in component of your defenses, not just a dietary protein that happens to interact with your immune system.[3]

Helaina's effera™ is revolutionizing supplements with the first human-equivalent lactoferrin. Research shows better bioavailability and reduced immune response compared to bovine sources.
Once released, lactoferrin does several things simultaneously. It binds free iron at the infection site, cutting off the iron supply that bad bacteria need to grow. It directly disrupts the surface membranes of certain bacteria and viruses. And it signals to other immune cells, helping recruit reinforcements and coordinate the broader response.[4]
Researchers have also found that lactoferrin interacts with a molecular alarm system on the surface of immune cells called toll-like receptor 4 (TLR4). You can think of TLR4 as a sensor that recognizes bacterial signatures and fires off an inflammatory response when it detects them. Lactoferrin can interfere with that trigger, which helps prevent excessive or runaway inflammation when it isn't warranted.[5]
This is a critical distinction. Lactoferrin lactoferrin activates, rather than overactivates, your immune system, helping calibrate the response so it fires appropriately rather than chronically. Anthony Clark unpacks this biology from first principles in the PricePlow Podcast Episode #180 with Dan DeMarino and Anthony Clark, which is worth a listen if you want the full conceptual framework.
What Human Research Shows About Inflammation
Moving from mechanism to evidence: what does lactoferrin actually do to inflammatory markers in real people?
-
The Cytokine Evidence
Berthon et al., 2022 published a systematic review and meta-analysis examining lactoferrin's effects on inflammation, immune function, and respiratory infections in humans.[6]
effera™ human-identical lactoferrin demonstrates no alloimmune response in groundbreaking clinical trial, while bovine lactoferrin triggered antibody responses in over 50% of participants. First study to definitively answer the alloimmunization question for precision-fermented proteins.
The most consistent finding: lactoferrin supplementation at around 200mg per day reduced circulating IL-6 by an average of 24.9 pg/mL compared to controls. That matters because IL-6 is upstream in the inflammatory cascade. It's the signal that tells your body to mount a full-scale inflammatory response and, as established in the first article, it's the same signal that drives excess hepcidin production and locks down iron. Bringing IL-6 down touches both systems at once.
-
Cytokine Balance in Preclinical Studies
Beyond IL-6, lactoferrin also influences other key inflammatory signals. Hayashida et al., 2004 studied oral lactoferrin in a rat model of adjuvant-induced arthritis, a well-established research model for studying joint inflammation. The researchers found that lactoferrin suppressed production of tumor necrosis factor-alpha (TNF-α, a pro-inflammatory cytokine that drives tissue damage across many inflammatory conditions) while simultaneously increasing production of interleukin-10 (IL-10, an anti-inflammatory cytokine that helps calm and resolve immune responses).[7]
That shift in the ratio (less TNF-α, more IL-10) can move the needle in terms of well-being. Lactoferrin isn't simply quieting the alarm. It's moving toward meaningful resolution rather than perpetuation, nudging the immune system back toward balance. Similar findings were documented in a separate collagen-induced arthritis model, where oral lactoferrin significantly reduced joint inflammation markers.[8]
-
The Iron-Immunity Connection in Real Patients
We went behind the scenes at Helaina's Manhattan lab to see how they make human-identical effera™ lactoferrin through precision fermentation.
The most direct clinical evidence linking lactoferrin's anti-inflammatory action to improved iron outcomes comes from Lepanto et al., 2018, an interventional study in pregnant women diagnosed with anemia of inflammation. This is a condition where chronic inflammation, rather than simple dietary deficiency, is the underlying driver of low iron status. The body has enough iron, but it's being locked away by elevated hepcidin.[9]
After 30 days of lactoferrin supplementation, these women showed significant decreases in both serum IL-6 and hepcidin levels. Ferrous sulfate, the standard iron supplement given to the comparison group, produced no change in either marker.
This is the two-way street in clinical practice. By supporting a healthy IL-6 response, lactoferrin helped lower the hepcidin signal that was blocking iron from circulating. With hepcidin down, iron could move freely again. The intervention addressed the upstream cause rather than trying to force more iron through a system that was actively resisting it.
Lactoferrin and Your Immune Cells Directly
Beyond its effects on inflammatory proteins, lactoferrin also acts directly on specific immune cells: the specialized cells that execute your body's defensive responses.
-
Dendritic Cells and Antiviral Defense
Van Splunter et al., 2018 ran a nutritional intervention study in healthy elderly women and measured how lactoferrin affected a specialized type of immune cell called a plasmacytoid dendritic cell. These cells act as scouts that bridge your body's immediate, non-specific immune response and its longer-term, pathogen-specific defenses. They're especially critical for detecting viruses.[10]
Laura Katz and Pamela Besada-Lombana take us inside Helaina's Manhattan R&D facility to reveal the precision fermentation science, clinical breakthroughs, and empathy-driven culture behind effera® lactoferrin on Episode #197 of the PricePlow Podcast.
The study found that lactoferrin enhanced these cells' ability to respond through a viral recognition pathway called TLR7 (toll-like receptor 7, essentially your body's built-in virus detector). In older adults, this type of innate immune signaling naturally weakens with age. Lactoferrin supplementation improved the responsiveness of this pathway, which could meaningfully support antiviral defense in an aging immune system.
-
T-Cell Activation
Dix and Wright, 2018 examined how lactoferrin supplementation affected T cells, the immune cells responsible for coordinating your body's targeted responses to specific threats, and for remembering pathogens you've encountered before.[11]
In this pilot study, supplementing with 200mg of lactoferrin produced a statistically significant reduction in a T cell activation marker called CD69+ on helper T cells (CD4+ cells, which direct other immune cells and coordinate the broader immune response). In plain terms, CD69+ is a flag that appears on T cells when they're actively engaged in fighting something. A lower CD69+ reading in healthy, non-infected study participants suggests the immune system is operating in a more settled, less chronically activated state.
For someone dealing with ongoing low-grade inflammation (where the immune system is perpetually running warm without a clear acute threat), this kind of homeostatic calibration has practical value. At 200mg, this effect was statistically significant on CD4+ helper T cells.
Why effera® Changes the Calculus
Everything discussed so far applies to lactoferrin broadly, but we believe we can do even better thanks to modern technology, because the specific form matters. effera® is the first commercially available lactoferrin that's structurally identical to the human version.
Most lactoferrin supplements use bovine lactoferrin, derived from cow's milk. It shares roughly 70% amino acid sequence homology with human lactoferrin, meaning about 30% of the protein's building-block sequence differs.[5] Those structural differences affect how the protein folds, how it binds to receptors on immune cells, and how the body responds to it. It works, as shown by the evidence above, but does it work in our bodies as well as human lactoferrin?
-
Helaina's Preliminary Efficacy Data
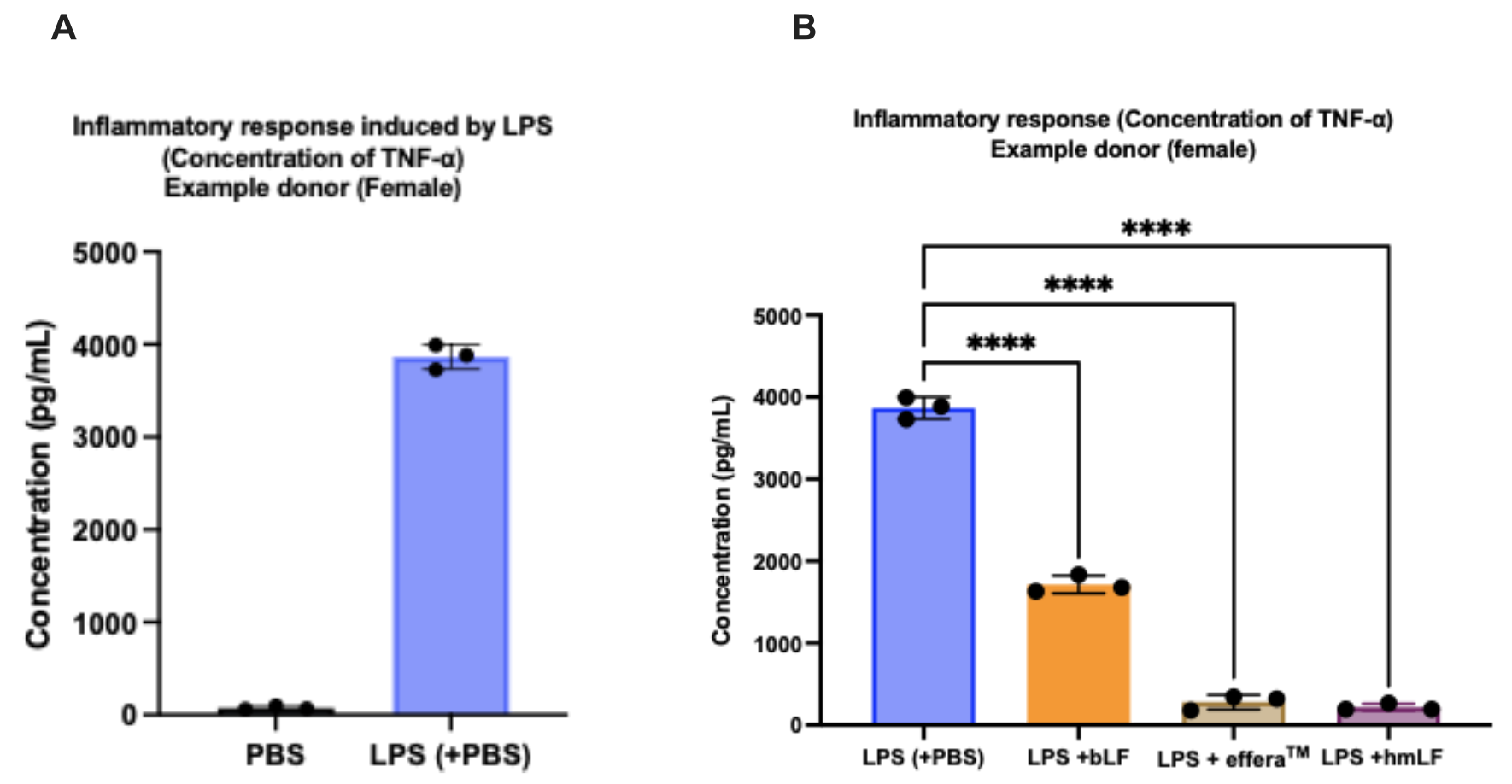
Helaina has run functional testing on effera® using peripheral blood mononuclear cell (PBMC) assays. PBMCs are immune cells drawn from human blood: a mix of lymphocytes and monocytes, which are central to immune response. To trigger an inflammatory response, researchers used LPS (lipopolysaccharide), a bacterial surface molecule that activates immune cells through the same TLR4 pathway discussed above.
Panel A shows how LPS spikes TNF-α in immune cells with no lactoferrin present. Panel B compares all three lactoferrin forms head-to-head -- effera® and native human milk lactoferrin both drove TNF-α down to near-baseline, while bovine lactoferrin produced a more modest reduction.
The question being tested: does effera® reduce the TLR4-triggered inflammatory response, and if so, how much? Only donors whose immune cells responded to LPS stimulation were included in the analysis.
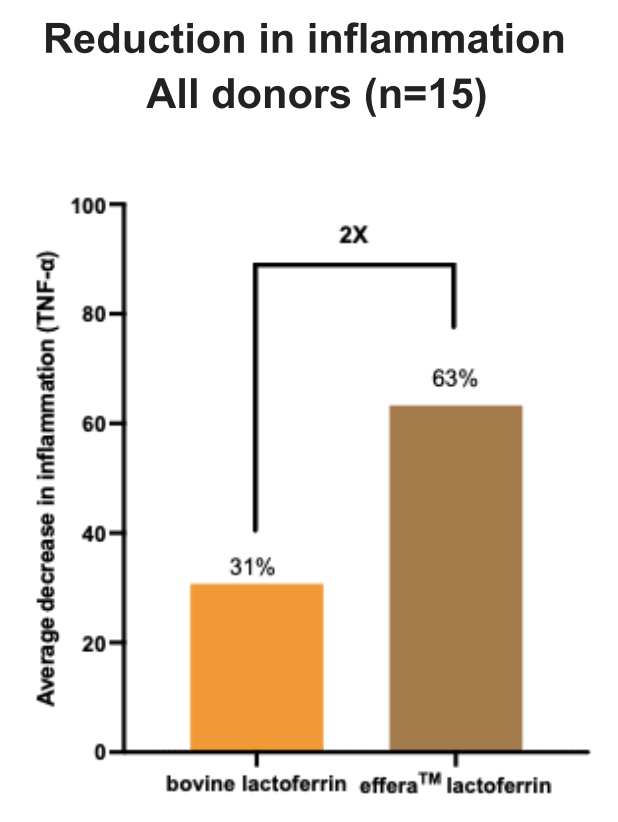
Over Twice the Effect of Bovine Lactoferrin
Using TNF-α as the measured output (the same pro-inflammatory cytokine from the Hayashida discussion above), effera® significantly reduced the LPS-induced inflammatory response in 12 of the 15 donors tested, with an average reduction of 63% across all responsive donors. Bovine lactoferrin, meanwhile, averaged a 31% reduction.
In Helaina's PBMC co-stimulation assay, effera® cut LPS-triggered TNF-α production by 63% across 15 responsive donors -- roughly double the 31% reduction seen with bovine lactoferrin.
That's just over double the effect, and the difference between the two was statistically significant. Perhaps the most telling result: effera®'s performance closely matched lactoferrin isolated directly from native human milk. If you're trying to assess whether precision-fermented human-identical lactoferrin actually behaves like the real thing, that comparison is about as direct a confirmation as you can get in a cell-based model. Helaina is conducting additional studies to build on these findings.
-
The Immunogenicity Problem with Bovine Lactoferrin
There's also a more fundamental issue with bovine lactoferrin that doesn't get discussed enough. Because it's a foreign protein (structurally different from what your body naturally produces), your immune system can recognize it as "not self" and mounts an antibody response against it. That means immune resources get spent targeting the supplement itself, which works directly against the goal.
The Peterson et al., 2024 randomized, double-blind clinical trial tested this directly. Over 84 days, more than 50% of subjects taking bovine lactoferrin developed detectable antibodies against it. Subjects taking effera® showed no such immune response.[12]
An immune modulator that triggers an immune response against itself is a problem worth taking seriously. We covered this trial in depth in The Landmark Lactoferrin Trial That Changed Everything, and Laura Katz and Pam Besada-Lombana discuss what these results mean for effera®'s ongoing development on PricePlow Podcast Episode #197.
Practical Takeaways
A few things worth keeping in mind if you're supplementing with lactoferrin for immune support:
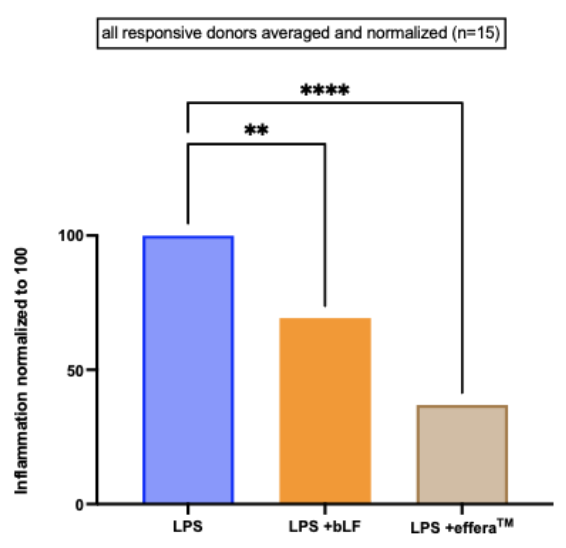
Averaged across all 15 responsive donors, effera® drove inflammation down to roughly 40% of the LPS-only baseline -- a statistically significant advantage over bovine lactoferrin, which landed near 70%.
- Dose range. Across the human immune trials reviewed here, 100mg to 200mg covers the effective range for immune applications. The Dix study found its strongest T cell effects at 200mg, and the Berthon meta-analysis centered on 200mg per day.
- Species matters. effera® does not elicit an immune response like bovine lactoferrin,[12] so some of the drawbacks seen with bovine lactoferrin may not apply. For instance, the Berthon meta-analysis found that bovine lactoferrin produced a better IL-6 reduction when taken before meals, but since human lactoferrin has better digestibility,[13] it's expected to perform better anytime it's taken.
- Who benefits most from this angle. The immune-iron connection is most relevant for people with chronic low-grade inflammation, older adults looking to maintain antiviral immune responsiveness, women with recurring iron issues that haven't resolved with standard supplementation, and athletes training hard enough to sustain elevated baseline inflammation year-round.
Two Systems, One Solution

Dan DeMarino and Anthony Clark from Helaina dive deep into precision fermentation technology and effera™ human-equivalent lactoferrin, revealing how 5-week development cycles and machine learning models are revolutionizing bioactive protein production on Episode #180 of the PricePlow Podcast.
The throughline across both articles in this series is consistent: your body regulates iron and immunity through shared signals, not isolated ones. When those signals get disrupted by chronic inflammation, both systems suffer. Conventional iron supplements bypass this entirely, and most immune supplements don't touch iron regulation at all.
Lactoferrin operates at the regulatory layer where both systems meet. It modulates the cytokines that drive hepcidin elevation. It calibrates immune cell activation. It sequesters free iron at infection sites to starve pathogens. These aren't separate effects layered on top of each other. They're the same biology, working through the same protein.
effera® delivers that protein in the form your body is designed to use: human-identical, recognized by your immune system without triggering a foreign response, and backed by a growing body of clinical and functional data.
For a full look at the effera® story from the beginning, visit our effera® ingredient overview. We'll keep building this series as new data comes out, so sign up below to stay current.