Long gone are the days when the supplement industry offered little more than proteins, multivitamins, and pre-workout formulas. Though these cornerstone products remain extremely popular, the industry has taken a more concerted interest in overall health and wellness. People arguably put more emphasis on their health now than they ever have, and brands have adjusted accordingly, formulating products that accommodate this growing trend.
NuLiv Science: A Premium Ingredient Developer

NuLiv Science is a novel ingredient supplier with some fascinating patented plant extracts with research-backing.
NuLiv Science, one of the supplement industry's leading premium ingredient developers, is consistently at the forefront of innovation. Having grown into a full-range supplier and early-stage nutraceutical formulator, NuLiv Science has developed a wide array of patented ingredients over the years that pop up in a variety of supplements. A few are so ubiquitous that you've likely seen them before:
- AstraGin, one of the industry's premier bioavailability-enhancing agents
- Senactiv (formerly known as ActiGin), increases cellular energy and regeneration
- InnoSlim supports metabolic health, optimal glucose levels, and efficient fat-burning.
Never one to stay fixated on one type/variety of ingredients, NuLiv Science has jumped in on the growing awareness of skin health.
Introducing Astrion
Astrion is NuLiv Science's cosmeceutical ingredient that has been clinically shown to nourish and hydrate skin. Leveraging standardized, purified extracts of Astragalus membranaceus and Centella asiatica, Astrion increases collagen production, hyaluronic acid synthesis, and absorption of the compounds that form collagen and hyaluronic acid in skin cells. This not only increases the skin's overall health and wellness, but defends it against ultraviolet (UV) radiation and also attenuates a decline in age-related skin health.

A patented combination of Astragalus membranaceus and Centella asiatica extracts, Astrion provides skin rejuvenation and hydration through enhanced endogenous production of collagen & hyaluronic acid
In this post, we'll get into the mechanisms mediated by Astrion to play a central role in skin health. Then, we'll look at the clinical data supporting Astrion's skin-benefiting prowess, and talk about a few products that use it.
Before we get started, subscribe to PricePlow's Astrion news and product alerts so you know what's happening with the ingredient! If you're here looking for a supplement with Astrion inside, check out Ghost Glow.
Subscribe to PricePlow's Newsletter and Alerts on These Topics
Before diving into Astrion, we give a primer on skin health and mechanisms, covering collagen, hyaluronic acid, MMPs, common problems, and more. If you're well-versed on skin care, you can skip down to the Astrion Information area of this article.
Skin Health 101: Collagen, Hyaluronic Acid, and MMPs
In order to fully understand and appreciate what Astrion is capable of, let's first discuss the mechanisms it affects. The skin is made up of three separate layers, each of which houses different components, properties, and functions:
- The epidermis is the outermost layer of the skin and also serves as its initial barrier. It consists of keratinocytes (water barrier formation), melanocytes (control skin pigment and coloration), Langerhans cells (first-line defenders), and Merkel cells (sensory cells).[1]
- The dermis contains the majority of the skin's connective tissues, sweat glands, hair follicles, blood vessels, and nerve endings.[1,2] In addition to housing fibroblasts, both collagen and elastin (two compounds that largely control skin health and function), are mainly produced in the dermis.[1,2]
- The hypodermis also stores connective tissues and blood vessels. However, this layer is mostly used to store adipocytes (fat cells).[1]
Each of these layers serves a specific purpose, though the epidermis and dermis largely dictate skin integrity and appearance. It's within these two layers of skin that a few major constituents are held and/or produced, including collagen, hyaluronic acid, and matrix metalloproteinases (MMPs).
Collagen
The extracellular matrix (ECM) is a non-cellular network of various collagens, proteoglycans, and glycoproteins that form a "structural scaffold" for cells.[3] It also houses key cytokines and growth factors that communicate cellular behavior. The ECM is central to skin health, integrity, and flexibility. As such, constituents that form the ECM are integral to skin, particularly collagen.
Collagens are the most abundant proteins in mammals, existing in 28 different forms across all vertebrates. These fibrous proteins have a triple-helix structure at their base, which allows them to form complex assemblies. In fact, structural complexity is what ultimately defines a collagen type — a triple helix forms roughly 96% of collagen I, whereas it builds only 10% of collagen XII.[4] Fibrillar collagens (types I, II, III, V) consist of only one triple helix and form striated fibrils.[5]
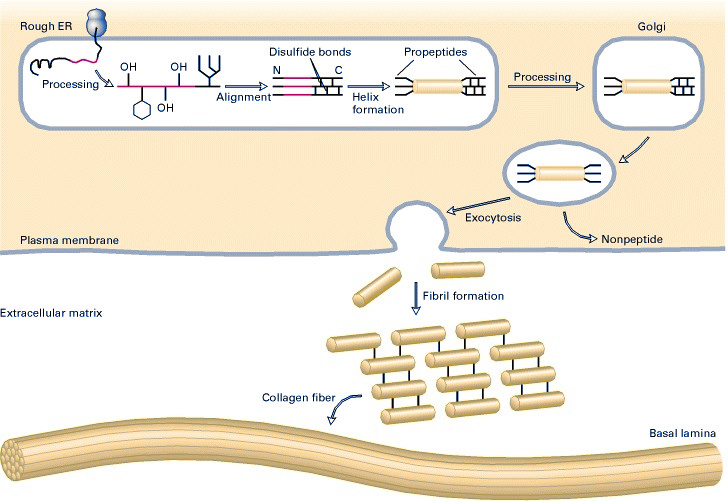
How is collagen formed?

Healthy skin comes from the inside as well as the outside. A major component is building strong collagen networks.
Collagen is a protein, which means it's built with amino acids. Three aminos (glycine, proline, hydroxyproline) form the basis for most helix structures. These structures can take one of two forms: either glycine-proline-X or glycine-X-hydroxyproline, where "X" represents any of the other 17 amino acids.[6]
Collagen is formed both in and outside of cells in humans. The intracellular process begins with the transcription of mRNA in the nucleus, which then moves to the endoplasmic reticulum. Once there, the polypeptide undergoes post-translational processing that forms pro-collagen — this consists of peptide removal, hydroxyl group additions to both lysine and proline residues (which requires vitamin C as a cofactor), and glycosylation.[6] Pro-collagen molecules move outside the cell, where collagen peptidases cleave propeptides and yield tropocollagen.[6] Finally, lysyl oxidase (a copper-dependent enzyme) induces covalent bonding that forms a collagen fibril.[6]
Collagen in humans
Only 16 types of collagen exist in humans, with collagen I, II, and III making up roughly 90% of total collagen content.[7] Collagen IV is important as well, but serves a very different role compared to the other varieties that exist alongside in the skin:
- Type I collagen fibrils form the basis of the skin, tendons, ligaments, fibrous cartilage, and connective tissues.[7] Type I collagen is tightly-packed and extremely strong, possessing more tensile strength than steel.[7]
- Type II collagen fibrils, which are both smaller and more loosely-packed than type I collagen fibrils, form the elastic cartilage that protects joints.[7]
- Type III collagen is mainly used to build muscles and organs, including the skin.[8,9]
- Type IV forms a two-dimensional reticulum that upholds tissue membranes and barriers.[10,11]
Types I and III are the primary types of collagen in the skin and are both formed and located primarily in the dermis.[9] Produced by fibroblasts residing in the dermal ECM, these collagens work alongside elastin (another protein formed in the dermis) to give skin the integrity and elasticity it needs to operate efficiently and protect the body.
Hyaluronic Acid

We've seen hyaluronic acid used in creams and serums, but what about making the body produce more on its own - from the inside?!
Hyaluronic acid (HA) is a glycosaminogylcan that is both produced and located in the ECM. Composed of repeating D-glucuronic acid and N-acetyl-D-glucosamine units linked by glucosidic bonds,[12] HA attracts and retains water molecules in the body.[12] This capability is highly important in the skin (where roughly 50% of all HA is located), though it's useful elsewhere, too. Hyaluronic acid is found throughout the body, including the eyes, synovial fluid, muscle tissue, heart, and lungs.[12] In these areas, the substance is used to hydrate and lubricate joints, regulate tissue health, and monitor immune response.[12]
In the skin, both the epidermis and dermis hold HA, though the latter contains significantly higher concentrations of it.[12] HA synthesis in the dermis largely influences water balance, osmotic pressure, and skin stabilization.[12] It also influences HA production in the epidermis,[12] which helps pull water to the skin's surface to keep it hydrated and moisturized.
MMPs
While both collagen and HA are compounds vital to optimal skin health, matrix metalloproteinases (MMPs) reside on the other end of the spectrum. A member of the metzinc superfamily of zinc-dependent endopeptidases,[13] MMPs are enzymes involved in a number of biological processes, including cell proliferation and differentiation, cell apoptosis, and immune response.[14,15] MMPs are largely involved in the ECM, where they facilitate protein degradation.[15]
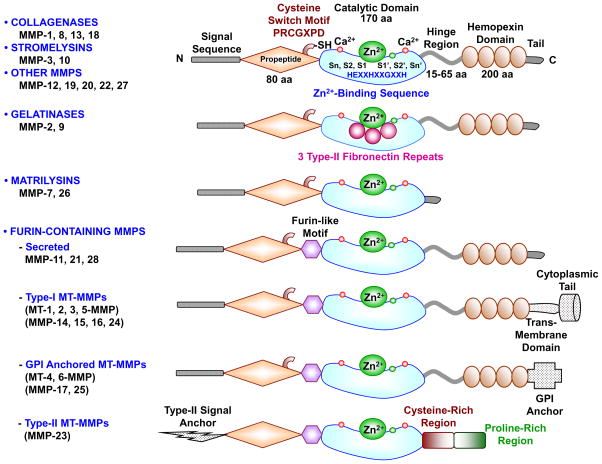
Most MMPs share a similar structure — a propeptide, a catalytic metalloproteinase domain, a linker peptide, and a hemopexin domain.[15] They are also secreted naturally by various tissues and cells, including fibroblasts and endothelial cells.[15] Science has identified 28 different MMPs in the body, which are grouped based on their substrate specificity and domain structure:
- Collagenases: MMP-1, MMP-8, and MMP-13
- Gelatinases: MMP-2, MMP-9
- Stromelysins: MMP-3, MMP-10, MMP-11
- Matrilysins: MMP-26
- "Membrane-Type" (MT): MMP-14, MMP-15, MMP-16, MMP-17, MMP-24, MMP-25
- Seven other MMPs that don't fit a specific subgroup[15]
The various characteristics shared among each subgroup dictate their action in the body. Collagenases, especially MMP-1, do as their name suggests — their primary function is degrading fibrillar collagen.[16] Though a few other MMP groups — gelatinases, matrilysins, and MT — facilitate collagen turnover to some degree,[16] collagenases eat away at the collagen that builds the skin.
MMPs have traditionally been viewed as enzymes that prevent optimal ECM health,[14] though that's not necessarily true. Advancing literature suggests that an effective balance between MMP and tissue inhibitors of metalloproteinases (TIMPs) activity regulates not only ECM function but most MMP-related processes.[15] Therefore, while MMPs do damage overall collagen health, we can't simply look to subdue these enzymes at all costs. However, limiting their activity while maintaining a healthy MMP/TIMP balance can keep collagen integrity high.
Declining skin health
While there is certainly more happening inside the skin that involves other compounds, these three constituents are largely important to its overall health. Collagen forms the basis of the skin, upholding its strength and flexibility. HA is responsible for hydrating the skin, pulling and holding water in its outer and middle layers. MMPs, on the other hand, degrade the proteins the skin needs to function properly. Thus, high-volume production of collagen fibrillar and HA, alongside limited MMP activity, helps keep the skin happy and healthy. This not only means strong, moisturized skin, but also skin that is largely wrinkle-free, properly colored, and supple.
Of course, healthy, nourished skin doesn't last forever. The biggest culprits of declining skin health are aging (intrinsic and extrinsic) and ultraviolet (UV) radiation exposure.
Aging
As the human body ages, its capabilities and operational efficiencies decline. In regards to skin, the three aforementioned components of skin health are all affected by aging:
- Collagen production decreases, fibril strength declines, and degradation and fragmentation increase[17]
- Increases in HA avidity with tissues induces decreases in epidermal and dermal HA content, though the former sees a significantly larger drop-off[12]
- MMPs facilitate ECM remodeling, which not only influences skin health, but also the potential development of age-related disease.[18]
While such changes are seen in intrinsic aging — the "natural", unavoidable aging process — they're also encouraged by extrinsic aging. Lifestyle choices such as poor nutrition,[19] smoking,[20] and exposure to high levels of stress are external factors that can alter skin appearance and make it look older than it actually is.[21] The similarities in skin appearance brought on by intrinsic and extrinsic aging are explained well at the molecular level — both are related to high oxidative stress, DNA damage, telomere shortening, microRNA alteration, accumulation of advanced glycation end products (AGEs), and inflammation.[19]
UV Exposure
Though technically a means of extrinsic aging, UV exposure is so influential in terms of skin health that we thought we'd discuss it separately.
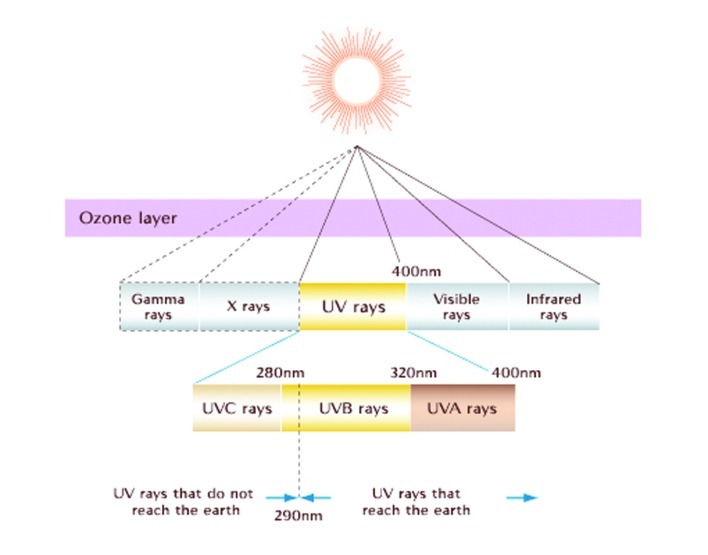
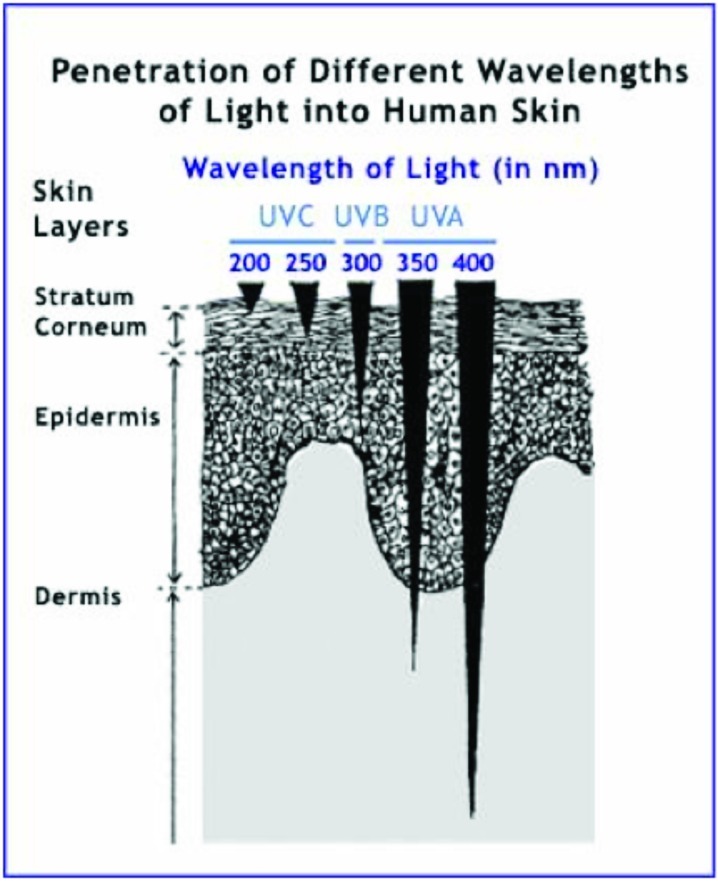
Typically, humans are exposed to UV through sunlight, which emits all three types of UV radiation — UVA, UVB, and UVC.[22] The earth's ozone layer blocks UVC from reaching its surface, leaving UVA and UVB as the UV radiation that penetrates the skin.
UVA rays get deeper into the epidermis and dermis than UVB rays, due to having a larger wavelength. And while UVB rays can be more damaging, they aren't as prevalent as UVA rays — roughly 95% of the UV that hits the earth's surface are UVA.[23] These rays can be problematic, especially in terms of skin health.
According to a review published in the Journal of Clinical and Aesthetic Dermatology in 2012, chronic UV exposure encourages premature skin aging, decreases immune response, and can lead to potential gene mutations and skin cancers.[22] Artificial implements, such as tanning beds, are also known to emit UV radiation.[22,24] Using sunscreen is often suggested as the primary means of protecting oneself from excess UV ray exposure.
All that being said, UV radiation isn't totally harmful. UV rays modulate the natural synthesis of vitamin D,[25] a vital nutrient that the human body needs. They can also be used as a means of treating specific conditions and diseases, such as depression and psoriasis.[22] Despite a complex array of influence on humans, though, UV radiation is generally spoken of in light of its damaging effects on the skin. In regards to collagen, hyaluronic acid, and MMP activity:
- In a 2013 study published in Biopolymers, researchers used circular dichroism experiments to display that UV radiation induces photodegradation of collagen fibrils. [26] However, it's important to note that this study used UVC rays, exclusively
- In 2018, a study in BioMed Research International saw that a hyaluronic-acid-based formulation reduced UVA-mediated damage and oxidative stress.[27]
- An in vivo procedure, published in a 2001 edition of the Journal of Investigative Dermatology, found UV radiation to increase collagenase activity.[28]
Melanin - controlling UV sensitivity
Melanin content in the epidermis modulates the body's response to UV radiation. Melanin is a term used to describe the three molecules that control UV sensitivity and skin pigmentation in humans — eumelanin, pheomelanin, and neuromelanin.[29] Of these tyrosine-based compounds, eumelanin is the most effective at blocking UV photons — thus, the more epidermal eumelanin one has, the more capable they are of withstanding UV exposure.[25,29]
Skin pigmentation is largely controlled by the ratio of eumelanin (brown-black) to pheomelanin (yellow-red) in the melanosomes that reside in the deeper part of the epidermis.[29] Higher amounts of pheomelanin results in pinkish skin, such as that seen in human lips.[29] Additionally, darker skin tends to be more dense with melanosomes, resulting in elevated melanin concentrations.[29]
To gauge how tolerant an individual is to UV radiation, scientists have developed the Fitzpatrick Scale. This scale categorizes individuals into one of six phototypes based on complexion, melanin levels, UV-induced inflammation, and cancer risk.[25] The higher the melanin levels, the less prone someone is to sunburn, skin inflammation, and skin cancer.[25]
The amount of melanocytes decreases with age, resulting in less epidermal melanin and pigmented "age spots".[30] Reduced melanin levels are desirable in some cases, particularly in instances where one is chasing fairer, lighter skin.
Astrion: Encompassing Regulator of Skin Health

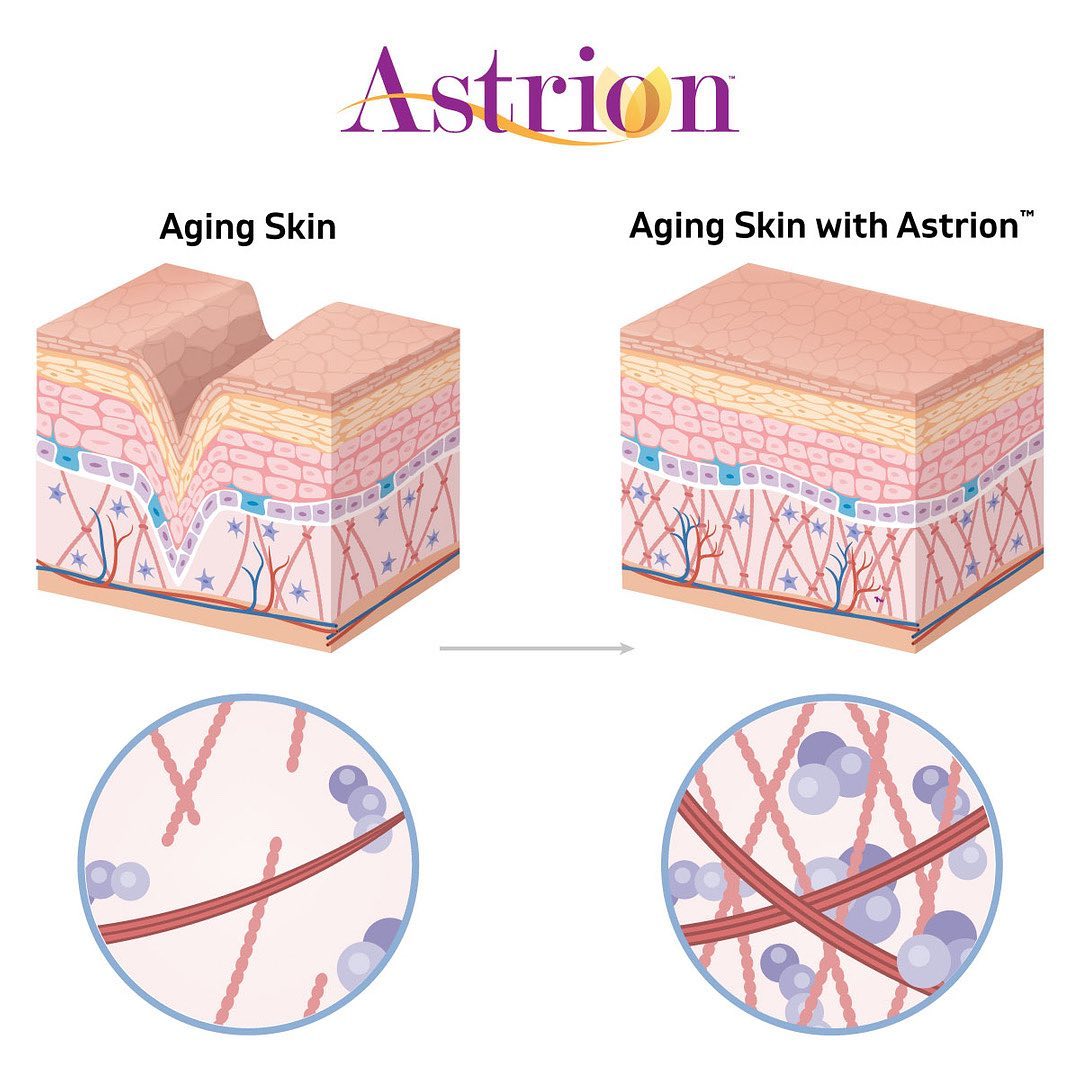
Astrion: A patented combination of Astragalus membranaceus and Centella asiatica extracts that provides skin rejuvenation and hydration via enhanced collagen and hyaluronic acid production
Collagen, hyaluronic acid, and MMPs largely dictate overall skin health, with melanin also contributing to the skin's color and sensitivity. Factors such as aging and UV exposure affect skin as well by acting on these underlying compounds. If the characteristics of healthy skin — potent collagen integrity, high HA content, depressed MMP activity — fall out of balance, the skin becomes susceptible to wrinkles, dehydration, discoloration, and even cancer.
Astrion from NuLiv Science aims to prevent such issues. This patented[31] ingredient leverages highly purified extracts of Astragalus membranaceus and Centella asiatica — two medicinal herbs that have been used in folk medicine for centuries — to intervene and help these compounds that lie within the skin. Astrion has been shown to increase collagen production in both the epidermis and dermis, increase epidermal HA synthesis, and decrease MMP expression. These capabilities actively fight against skin aging and UV exposure, resulting in nourished, radiant skin that looks healthier and younger.
The bioactives behind Astrion
The potency of Astrion is dependent on the primary bioactive compounds in each of its extracts.
-
Astragalosides
NuLivScience is a global research company with several patented ingredients including AstraGin, InnoSlim, and Senactiv on top of Astrion
Astragalosides (AST) are a group of triterpenoid saponins found in Astragalus membranaceus that provide benefits in a wide range of applications— these glycosides have been shown to act as antioxidants, antiasthmatics, and immunoregulatory and cardioprotective agents. They're also capable of supplying neurological benefits via crossing the blood-brain barrier.[32]
There are four astragalosides, categorized by Roman numerals (I-IV). Most research revolves around a comprehensive astragalus extract that delivers a full profile of astragalosides. There are also a few studies that use specific glycosides to propose astragalus as a skin health-promoting agent.
In a 2014 study published in Molecular Medicine Reports, researchers tested the effects of AST IV on various markers of photoaging in human skin fibroblasts (HSFs). Specifically, they measured the compound's ability to induce transforming growth factor-β (TGF-β), a key regulator of collagen synthesis, under the influence of UV radiation.
The study authors found that AST IV enhanced cell viability in HSFs while reducing cytotoxicity in UVA-irradiated cells.[33] Additionally, AST IV reversed UVA-induced inhibition of type I procollagen production,[33] effectively protecting against type I collagen degradation. The researchers also observed reduced MMP-1 expression in irradiated cells treated with AST IV. These effects were attributed to the extract's ability to attenuate negative factors in the TGF-β pathway that UVA and UVB radiation induce.[33]
Another study, published in the Journal of Pharmacy and Pharmacology in 2012, tested AST II on HSFs exposed to UVB radiation. Blotting and cytochemistry examinations conducted by the researchers showed that HSFs treated with AST II prior to UVB exposure were significantly protected from radiation compared to those that received no treatment — cell viability was 142.8% higher in the test group.[34] These cells also displayed significantly lower MMP-1 protein expression and higher type 1 procollagen activity compared to those that didn't receive AST II.[34]
Both of these studies also found AST treatment to be effective in cells that weren't exposed to radiation.[33,34] These experiments support AST's use for boosting skin health, as the compound acts on the molecular level to maintain collagen production and integrity.
-
Centella: Asiaticoside and other triterpenes
On the other hand, Centella asiatica supplies Astrion with asiaticoside. This pentacyclic triterpene is one of the few bioactive glycosides found in centella, but is often seen as the plant's main active constituent and is the component that full centella extracts are typically standardized for. Other compounds, such as madecassoside, have similar action, as well.
In a 2013 review published in Advances in Dermatology and Allergology, researchers analyzed the potency of centella extracts in applications related to the skin — wound healing, photoaging, and inflammation — and the underlying mechanisms behind them. They found that centella, driven mainly by asiaticoside and madecassoside, could:
- Increase total protein, collagen, and hydroxyproline (which is used to build collagen fibrils) content in wounds[35]
- Increase lysine and proline metabolism, effectively feeding collagen production[35]
- Stimulate hyaluronic acid production in wounds[35]
- Induce type I collagen synthesis in HSFs via TGF-β modulation[35]
These effects can be leveraged in a full centella extract. In a 2008 clinical trial from Experimental Dermatology, researchers gathered 20 female volunteers between 45 and 60 years old with photoaged skin. For six months, the volunteers applied a centella-containing topical to their skin. At the conclusion of the study, the women experienced significantly improved skin firmness, elasticity, and hydration.[36]
Other studies have tested the herb in cases of cellulite (liposclerosis), a non-inflammatory change in adipose tissue that results in visible skin alterations. One particular study found that of 60 individuals with cellulite who applied a centella-based topical to their skin four times a day for four months, 85% showed significant improvements in cellulite attenuation and overall skin condition.[35]
Astrion Trials
NuLiv Science has funded 12 in vitro studies and one clinical study testing its potent skin-boosting ingredient. The results seen in vitro on human fibroblasts are eye-catching:
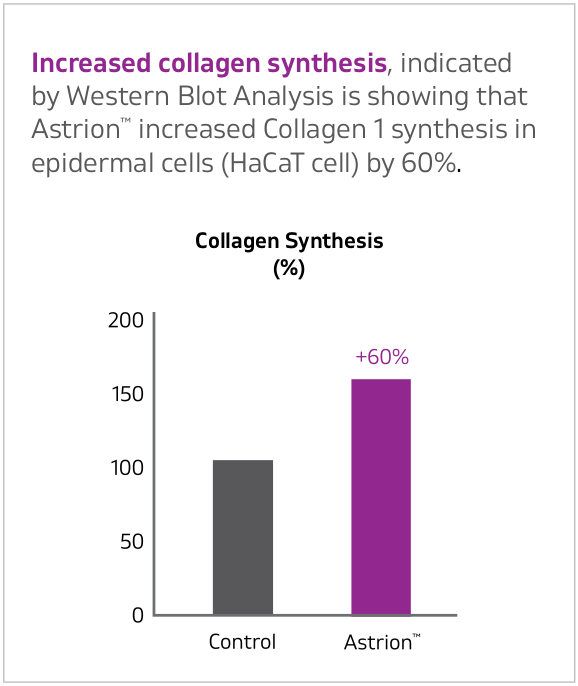
- 60% increase in type I collagen synthesis in epidermal cells
- 80% increase in type I collagen synthesis in dermal cells
- 45% increase in type I collagen secretion in dermal cells
- 30% and 80% increases in type III collagen synthesis and secretion, respectively, in dermal cells
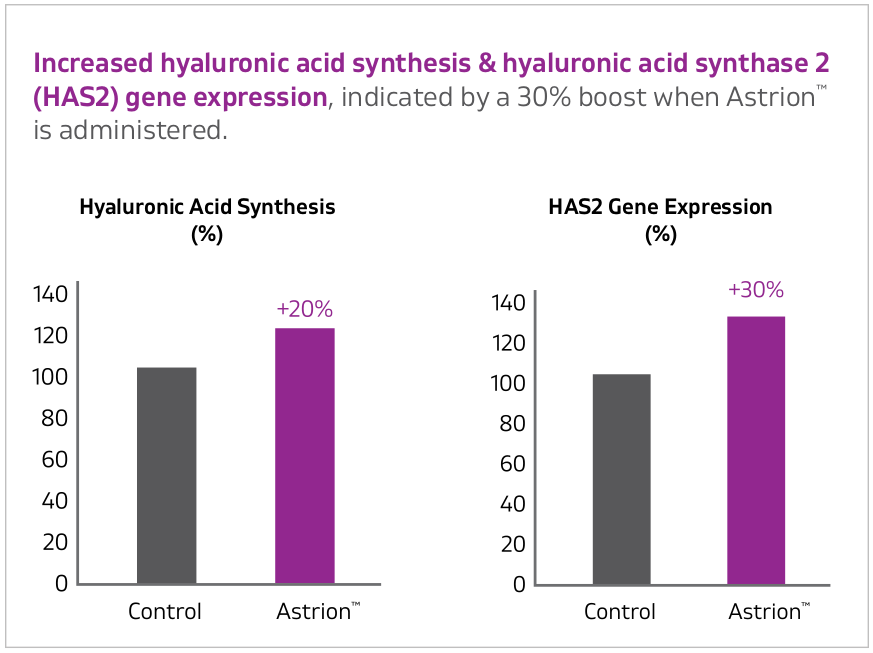
- 20% boost in hyaluronic production in epidermal cells
- 30% rise in hyaluronic acid synthase expression in epidermal cells
- 27% and 11% increases in proline uptake and glucosamine uptake, respectively, in epidermal cells
- 265% rise in telomerase activity in epidermal cells
- Roughly 50% decreases in MMP-1 synthesis and gene expression in dermal cells[37]
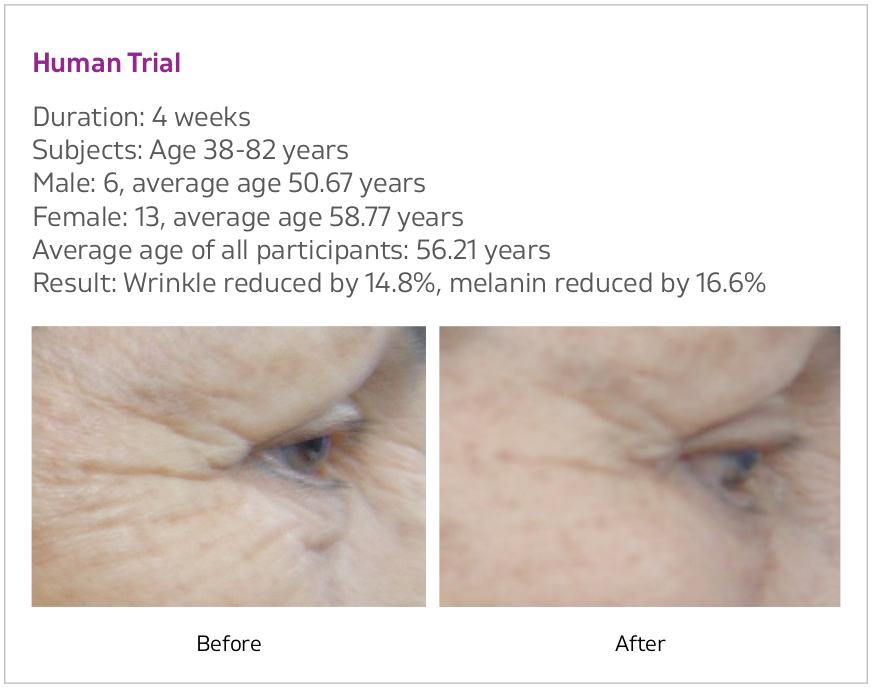
In the clinical trial, 19 volunteers between ages 38 and 82 used Astrion for four weeks. At the conclusion of the study, the subjects reduced the appearance of skin wrinkles by 15% and melanin by 17%, displaying visibly smoother skin while diminishing discolorations and the appearance of characteristics like sunspots.[37]
Application process
Astrion can be taken both orally or topically, a versatility provided through its active components. Both extracts are driven by triterpenoid saponins. The molecular structure of these compounds contains a lipophilic group and a hydrophilic group. This allows Astrion multiple means of reaching the inner-workings of the skin — transcellular passage, diffusion, passage through the stratum duct or transfollicular, or movement through sweat ducts.[37]

On this site, we generally talk about supplements ingested orally (such as Ghost Glow), but Astrion can also be used topically!
This transdermal effect allows Astrion to act on both epidermal and dermal cells, ultimately stimulating the synthesis of collagen, hyaluronic acid, and the other underlying mechanisms that affect skin health.
Astrion Safety and Dosage
Ingredient Safety
Both Astragalus membranaceus and Centella asiatica, the two active extracts in Astrion, are very safe ingredients. Astragalus has been tested at massive daily doses (60 grams per day for four months!) without causing any adverse effects.[38]
Though such extremes haven't been taken with centella, it too seems to be rather safe. One 2005 study did observe jaundice and liver inflammation in three women taking the herb — however, neither the ingredient quality or dosage were disclosed.[39] Most clinical trials have used between 250 milligrams to 500 milligrams of a standardized extract without seeing adverse effects.[40] Centella seems to be pretty well-tolerated in most cases, though further research on potential hepatotoxicity is needed before its safety is truly cemented.
Astrion Dose
Studies provided by NuLiv Science suggest two different doses based on the ingredient's form. Topicals should contain at least 5% Astrion, while oral doses should amount to a daily 250 milligrams. These relatively small doses are beneficial in terms of practicality, too. Not only does the size make it easy for consumers to get the ingredient in on a daily basis, but it also makes it easier for formulators to include it alongside other ingredients in a larger formula. An effective, efficient ingredient that doesn't take up a lot of space is music to their ears — they can use it without having to sacrifice other potential inclusions, elevating their overall formula.
Astrion is a relatively new ingredient, but we've actually seen it already in one of our favorite health and wellness formulas. Ghost Glow, Ghost Lifestyle's 2020 awesome entrant into the skin care space, packs a 250-milligram dose of Astrion to help deliver radiant, healthy skin. Even after altering the formula slightly in their Nana Berry flavor collaboration in 2021, Astrion remained untouched, showing just how central it is to the overall product.
Astrion Pushes the Skin Health Market Further
Overall health and wellness consists of an almost endless array of different areas, most of which go unnoticed to the naked eye. Skin health, however, does not — it's often one of the first things you can see!
The visibility and importance of skin quality has led to the formulation of ingredients/supplements that can help support it. NuLiv Science, which boasts an extensive profile of ingredients that are among the industry's best, developed Astrion to do just that. Using high-quality, purified extracts of Astragalus membranaceus and Centella asiatica, this ingredient has been clinically shown to improve multiple markers of skin health — elevated collagen synthesis, increased hyaluronic acid production, decreased MMP expression. Additionally, human trials have seen the ingredient reduce wrinkles and improve skin discoloration.
As consumers look for means to support the health of their skin and chase skin rejuvenation, Astrion from NuLiv Science presents one of the industry's most innovative, potent ways of doing so. When choosing your next skincare supplement, make sure to take a look at the label to see if Astrion is included!
You can see our other related content and sign up for news alerts on our NuLiv Science page.





Comments and Discussion (Powered by the PricePlow Forum)