Prostate health is something that young men probably don't think about at all, but we older, wiser, and more refined gentlemen think about it far more frequently. That's because prostate conditions are common as we age – one third of men have benign prostate hyperplasia (BPH) by age 50, and 90% of men have it by the time they're 85.[1]
Whether you're young and hoping to prevent prostate issues, or old and looking to manage them, we have an exciting new supplement for you to consider trying.
Jam-packed with big servings of powerful, research-tested ingredients for prostate health and overall male endocrine health, Core PROSTATE from CORE Nutritionals is formulated to keep your hormonal health optimized, and your prostate the appropriate size. This is part of the Core Lifeline Series launched towards the end of 2021, with formulas all similarly packed and uniquely designed to assist with different organ systems or goals.
Before we dig in, see PricePlow's coupon-powered prices and sign up for our CORE Nutritionals news alerts, since they have a lot planned for the future:
Core Nutritionals PROSTATE – Deals and Price Drop Alerts
Get Price Alerts
No spam, no scams.
Disclosure: PricePlow relies on pricing from stores with which we have a business relationship. We work hard to keep pricing current, but you may find a better offer.
Posts are sponsored in part by the retailers and/or brands listed on this page.
This area is reserved for Team PricePlow's upcoming Ingredients video.
Subscribe to our channel and sign up for notifications so you catch it when it goes live!
A quick message on Benign Prostatic Hyperplasia
Of the lower urinary tract symptoms (LUTS) are obstructive and irritative symptoms. The obstructive ones include poor urinary flow, straining, incomplete urinary completion, or incontinence. The irritative ones include increased urination frequency, painful urination, and nocturia (awakening to go to the bathroom at night).[2]
Similarly, this article mentions prostate cancer and prostate specific antigen (PSA), a measure used to determine a man's risk of prostate cancer.[3]
As always, dietary supplements are never intended to cure, treat, or diagnose any disease, and you must seek your doctor's approval before starting new supplements.
However, many of the ingredients listed in this supplement have copious amounts of sound research indicating benefits as adjunct therapies alongside what your doctor recommends - which should include a anti-hyperinsulinemic diet that prevents insulin resistance (meaning a high-protein diet free of omega-6 vegetable oils and low in refined carbohydrates), since hyperglycemia and insulin resistance are highly-correlated to the incidence of these conditions.[4]
With that disclaimed, let's get started:
Core Prostate Ingredients
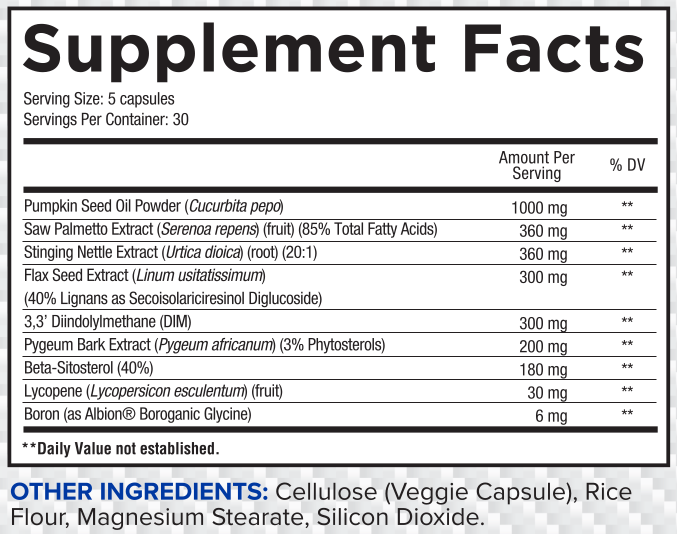
In a single five capsule serving of Core Prostate from Core Nutritionals, you get the following:
-
Pumpkin Seed Oil Powder - 1g
Core PROSTATE Ingredients, each one of them backed by science. 5 capsules per day, with or without food.
Pumpkin seeds are one of the few good plant sources of zinc, a mineral that's been described as the "master mineral of the male endocrine system". A 2011 study discovered that men with benign prostatic hyperplasia (BPH) eliminated more zinc through their urine, depleting their prostate of zinc in the process.[5] Partly because of this, pumpkin seeds have actually been used to prevent and treat BPH.[5]
Another study, this one published in 2009, found that combining pumpkin seed oil and saw palmetto oil (another ingredient in CORE Prostate) significantly reduced BPH symptoms.[6] Although more research is needed on this subject, the preliminary results indicate that this improvement was due to the anti-androgenic, anti-globulin, and anti-inflammatory activities of these compounds.[6] They may also beneficially alter cholesterol metabolism.[6]
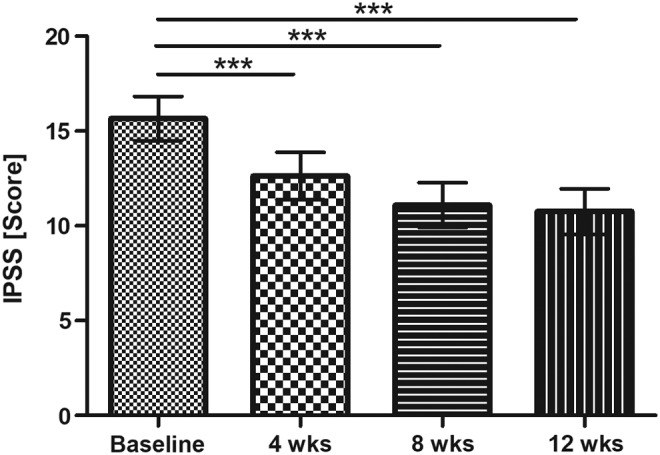
In a 2014 study, researchers gave BPH patients either 500 mg of pumpkin seed extract or a placebo for 12 months. After a year, the scientists measured the severity of the patients' BPH symptoms using the international prostate symptom score (IPSS), and found that pumpkin seed extract significantly reduced symptoms of BPH compared to placebo.[7] Not only was this study randomized, double-blind, and placebo-controlled – the "gold standard" study design in medical research – but it also had a fairly large sample size, with over 1,400 participants between the ages of 50 and 80 years old,[7] so the results are unlikely to be spurious.
After just one month, pumpkin seed extract significantly reduced IPSS score, and it continued to get better over the next two months![8]
In a smaller study from 2019, researchers took 60 males with an average IPSS score of 14.8, which is pretty high, and instructed them to take pumpkin seed extract once per day before going to sleep.[8] Before starting the regimen, the patients had their frequency of nocturia (going to the bathroom at night) and residual urine levels[8] measured by the researchers. After 12 weeks of taking pumpkin seed extract, the frequency of nocturia and the bladder emptying of the patients was significantly improved, leading to a boost in overall quality of life.[8]
One last thing to note about pumpkin seed extract is that it can potentially inhibit a specific type of prostate hyperplasia that's caused by the combination of testosterone and prazosin, a common blood pressure medication[9] – so if you are taking prazosin, pumpkin seed extract might be worth researching as a prophylactic. As always, talk to your doctor before starting any supplementation regimen - especially if using pharmaceutical drugs.
-
Saw Palmetto Extract (Serenoa repens) (berry) (Std. to contain 85-95% Fatty Acids & Sterols) – 360mg
Saw palmetto, also known as Serenoa repens, is a kind of palm tree native to the southern United States. Extracts, teas, and supplements derived from saw palmetto have become popular in recent years because of its beneficial effects on the male endocrine system.
Discussed below, saw palmetto has enough evidence across multiple studies showing improved symptoms of BPH, and that's what was known in 1998.[13]
Saw palmetto extracts are standardized for the fatty acids and sterols that occur naturally in the plant – examples being beta-sitosterol, caprylic acid, oleic acid, and palmitic acid, along with some lipases (digestive enzymes that break down dietary fats), tannin, and carotenoids (antioxidant vitamin A precursors), all of which contribute to its positive effects.[10]
As you can see from the Core Prostate label, Core Nutritionals is using a highly potent extract, standardized for 85% bioactive compounds.
Multiple studies have shown that saw palmetto extract supplementation improves prostate health, urinary tract issues, hair loss, testosterone production, and systemic inflammation.[10-12]
The 18-study meta-analysis
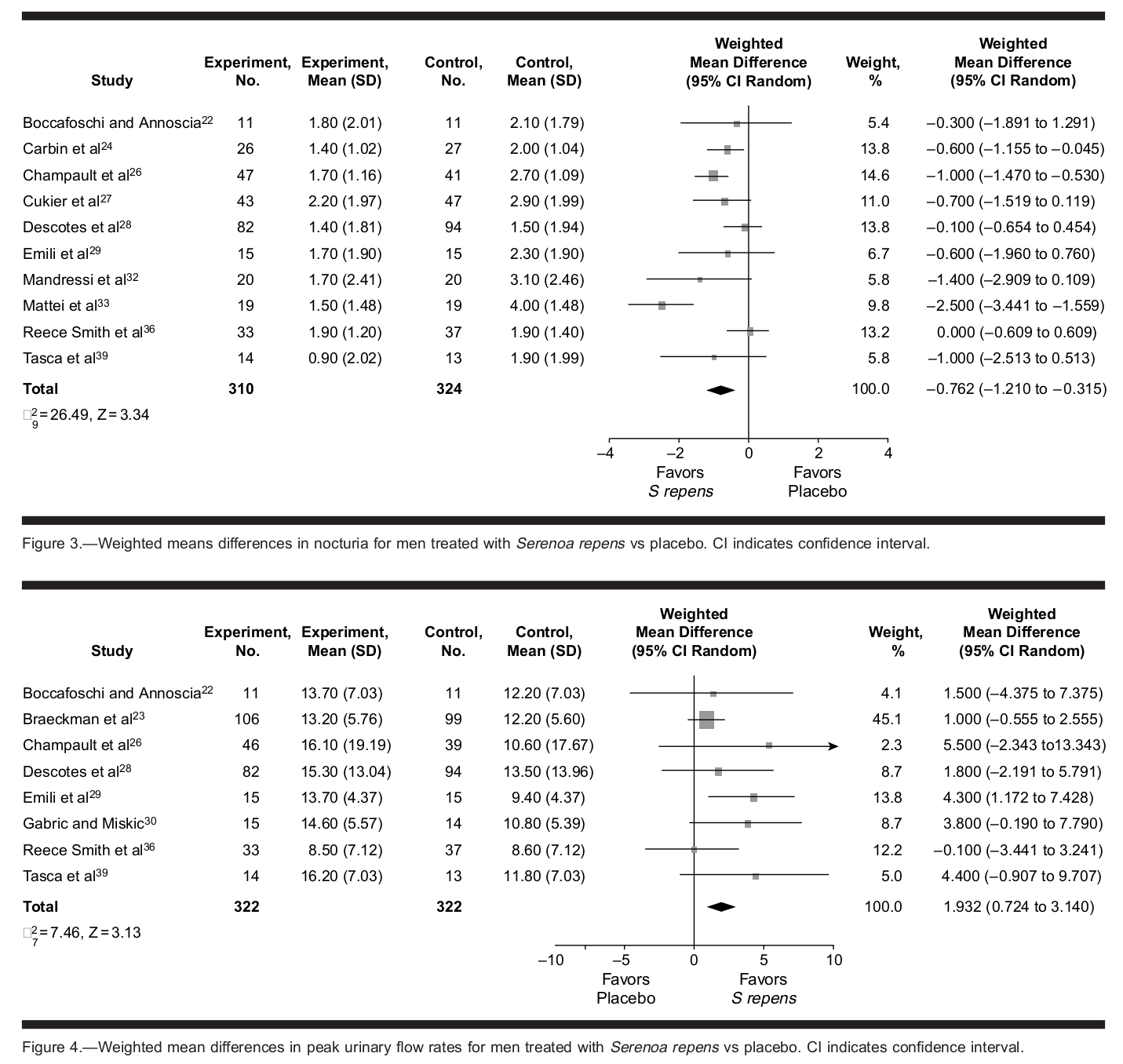
But if that wasn't enough for you, get this: a meta-analysis of 18 different randomized, double-blind, placebo-controlled studies, with a collective sample size of over 3,000 men, found that taking supplements from Serenoa repens significantly improved urinary tract symptoms, reduced nocturia frequency, and increased urinary flow.[13] Compared to finasteride, an accepted and proven urinary tract medication, saw palmetto did just as well at improving urinary flow and urinary tract symptoms, but with fewer adverse effects.[13]
A 2001 study found that saw palmetto supplements significantly improved symptoms of lower urinary tract infections, compared to placebo.[11] However, in this study, saw palmetto was not observed to have any effect on urinary flow[11] – highlighting the fact that more research is needed in this area.
The 5-alpha reductase / DHT connection
Introducing the Core Lifeline series! With Doug Miller at the helm, this is an unsurprising move -- but wait until you see the dosages in these supplements!
Another thing to note about saw palmetto is that it's a potent 5-alpha reductase (5α-R) inhibitor.[10] 5α-R is the enzyme that converts testosterone into dihydrotestosterone (DHT), and elevated levels of DHT have been shown to be associated with hair loss, so in theory, reducing levels of DHT by supplementing with saw palmetto could potentially slow or prevent hair falling out.
But we're interested in reducing DHT because high DHT activity is associated with developing an enlarged prostate.[14]
Saw palmetto may even be able to discourage the growth of cancer cells in the prostate, because of its activity as a cyclooxygenase-2 (Cox-2) inhibitor,[12] although much more research is needed on this topic before definitive conclusions can be drawn.
Ultimately, we have a good, strong dosage of a trusted prostate-beneficial ingredient. Next, we have one that's been in various men's supplements, but not often targeted for prostate health:
-
Stinging Nettle Extract 20:1 (root) - 360mg
The incredible-looking Stinging Nettle (Urtica Dioica) plant with even more incredible effects. Image courtesy Wikimedia
Also known by its binomial nomenclature Urtica dioica, stinging nettle is a flower plant native to Europe, Africa, and parts of Asia that's long been used in traditional medicine to treat inflammatory conditions such as osteoarthritis and rheumatoid arthritis.[15] Although most parts of the planet seem to have one benefit or another, the one we're interested in is the root of stinging nettle, since that is the part of the plant that has been identified as having potential in the treatment of BPH[15] – and root extract is indeed what Core Nutritionals has opted to use in Core Prostate.
In a 2012 study, researchers found that stinging nettle extract, much like saw palmetto, is able to act as a 5-alpha-reductase (5α-R) inhibitor, thus preventing the conversion of testosterone to DHT and reducing the likelihood of developing an enlarged prostate.[16]
Another study from 2005 found that 18 months of supplementation with stinging nettle extract had beneficial effects on BPH symptoms.[17]
-
Flax Seed Extract – 300 mg
You might be surprised to see Flax Seed making an appearance in a men's health supplement, since it is traditionally used in women to positively modulate the balance of estrogen.
Core SOOTHE is a comprehensive inflammation support supplement that we recommend alongside PROSTATE, since inflammation is associated with prostate issues, as discussed in the conclusion of this article
Flax is rich in specific types of lignans that are converted by mammalian digestive tracts into "weak" estrogen metabolites[18] – "weak" here meaning weaker than endogenous mammalian estrogens, such as estradiol.
By occupying the estrogen receptors of your body's cells, these "weak" estrogens can displace "strong" estrogens, thus inhibiting the action of the latter, and lowering the functional estrogenic burden of the body.[18]
This anti-estrogenic action matters for male health, and prostate health specifically, because of the relationship between testosterone, estrogen, and BPH. A 2018 review of the research literature on BPH found that aromatization – the conversion of testosterone to estrogen – might be why there's a correlation between testosterone levels and BPH risk.[19]
Because "weak" phytoestrogens can inhibit the action of the strong estrogens produced by aromatization, the researchers conclude, phytoestrogens like the lignans found in flaxseed could play an important role in the management of BPH.[19]
-
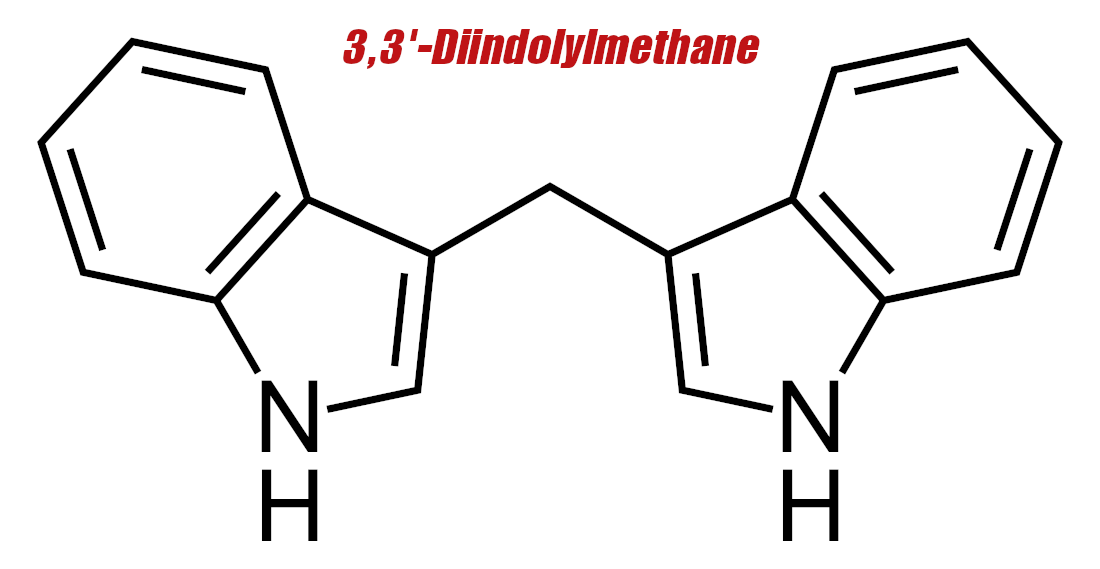
3,3'-Diindolylmethane (DIM) — 300 mg
Diindolylmethane (DIM) works by inhibiting the enzyme we were just discussing in the section about flaxseed above. To understand the action of DIM, first we need to delve a little deeper into what aromatase is and how it works.
Aromatase is responsible for converting androgens (testosterone and its metabolites) into estrogens. Although some estrogen is needed for optimal health in both men and women,[20] aromatase can easily become overexpressed, thus contributing to a syndrome called "estrogen dominance" – basically, too much estrogen – which is very bad news for anyone who has it. Aromatase overexpression has been associated in the research literature with several diseases, including some forms of cancer.[21] Obesity is one example of a common medical condition that can cause aromatase overexpression.[22]
DIM has been studied for its potential as an aromatase inhibitor, and has been show in preliminary studies to reduce the growth of estrogen-dependent breast cancer cells in vitro.[23] One theory as to DIM's anti-aromatase action is its affinity with the aryl hydrocarbon receptor (AhR), which downregulates estrogen receptors.[21,24,25] By stimulating AhR, DIM may help decrease estrogen's action in the body.[26]
But DIM doesn't just reduce the conversion of testosterone to estrogen – much like flaxseed, which we discussed above, DIM also changes the body's balance of estrogenic activity for the better, by converting "strong" estrogens to weaker estrogens.
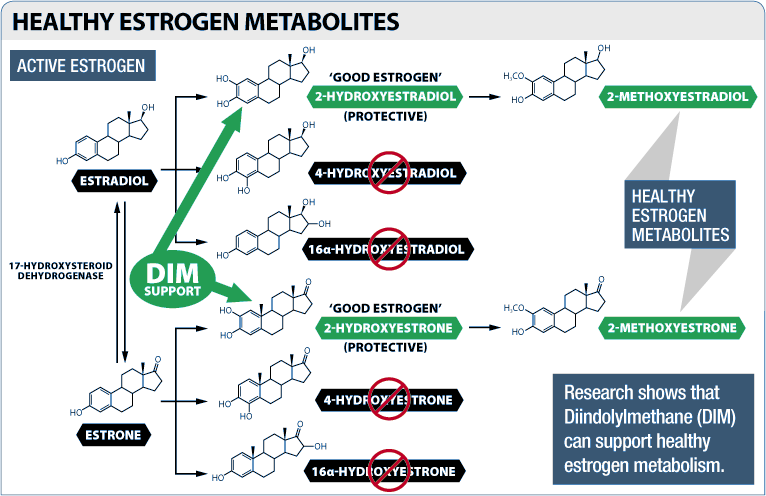
The human body produces three main forms of estrogen – estrone, estradiol, and estriol. Estradiol is the "strongest" of the three, meaning it has the highest activity at estrogen receptors[27] When these three estrogens are broken down, various estrogen metabolites are produced, among which are estradiol-2-hydroxylase (EH) and 16-alpha-hydroxyestrone.[27]
Researchers regard 2-hydroxylated estrogens as "good estrogens" due to their beneficial impact on human health,[28,29] and use the ratio of 2-hydroxylated metabolites to 16-hydroxylated metabolites as one measure of hormonal health. Having more "good" estrogen – a higher ratio of 2-hydroxlylated estrogen – is associated with higher levels of lean muscle mass and lower levels of fat mass.[30]
In 2012, a team of researchers found that by modulating enzymes which convert estrone to hydroxyestrones,[31] DIM increases the 2-hydroxylated (good) estrogen while decreasing 4-hydroxylated and 16-alpha-hydroxylated estrogens (which are bad).[31-34]
In other words, although it is not a phytoestrogen, DIM has effects that are similar to those of flax, modulating the body's estrogen metabolism in a way that might be favorable for the prevention and treatment of prostate disease.[19]
-
Pygeum Bark Extract – 200 mg
Pygeum bark extract is derived from the Prunus africanum tree, also known as the "African cherry tree", and is used in traditional African medicine for supporting prostate health. As is so often the case, modern research is finding that there was some real wisdom in this traditional practice, since pygeum bark extract has been shown to displace about 60% of the body's DHT from the DHT receptors,[35] thus reducing the action of DHT. Reduced DHT action is good news for us, because – again – high levels of DHT are linked to prostate enlargement.[14]
A 2002 study corroborated this, finding that men with BPH who took pygeum bark extract were twice as likely to report an improvement in their symptoms as men who took a placebo.[36]
A research review from the same year reached a similar conclusion, indicating that pygeum bark extract improves urinary symptoms in those suffering from BPH.[37]
-
Beta-Sitosterol – 180 mg
Beta-sitosterol, is a phytosterol – a sterol that occurs naturally in plants – with a chemical structure that's almost identical to that of cholesterol.
Because of its similarity to cholesterol, beta-sitosterol is able to block the intestinal absorption of dietary cholesterol,[38,39] leading to lower LDL and triglyceride levels.[38-40] Moreover, beta-sitosterol blocks the expression of the HMG-CoA reductase gene, which results in decreased synthesis of cholesterol.[40]
Beta-sitosterol is among the sterols found in saw palmetto, which we discussed above. In fact, some researchers believe that saw palmetto's beta-sitosterol content is one reason why it's effective in the management of BPH.[41]
In isolation, beta-sitosterol has also been shown to act as a 5-alpha-reductase inhibitor[41,42] just like a couple other ingredients in this stack, meaning it can potentially protect against prostate enlargement by lowering DHT.
-
Lycopene – 30 mg
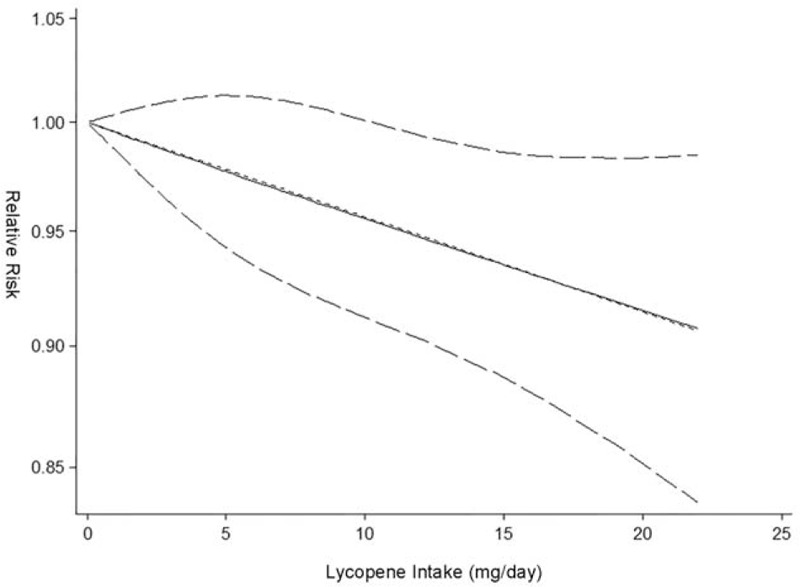
Dose–response analysis of lycopene consumption and risk of prostate cancer. The solid black line and 2 dotted black lines are the restricted cubic spline for the published relative risks (RR) and 95% confidence intervals (CIs).[49]
A classic mainstay ingredient for prostate health, lycopene is a carotenoid that occurs naturally in foods like carrots, tomatoes, watermelons, and grapefruits, giving them their reddish color.[43] Carotenoids are powerful antioxidants, and provide a multitude of health benefits, but getting a clinical dose from food would involve eating a lot of tomatoes, so most of us could potentially benefit from supplementing with lycopene.
A diet high in tomatoes has been linked to a lower risk of cancer – including prostate cancer.[43,49] Researchers believe this is primarily because tomatoes are high in lycopene, and a 2010 research review of 12 clinical trials concluded that there's an inverse correlation between lycopene intake and blood levels of prostate specific antigen (PSA), which is used to measure a person's risk for developing prostate cancer.[43]
-
Boron (as bororganic glycine) – 6 mg
Bororganic glycine is obtained from binding the mineral boron to the amino acid glycine. This makes the boron more bioavailable than boron alone.
It makes perfect sense that boron would boost testosterone, when you consider the fact that it looks totally badass. Image courtesy Wikimedia
Because boron both raises testosterone levels directly but also raises vitamin D levels,[44] boron is often used as a testosterone booster.
If you've been following the discussion so far, you'll probably realize that more testosterone is not necessarily better when it comes to prostate disease. But a small study from 2011 showed that boron supplements can reduce estrogen levels at the same time it raises free testosterone,[45] making it potentially useful in the management of BPH.
Additionally, raising vitamin D levels is potentially of some benefit for BPH, since vitamin D levels show an inverse relationship with BPH risk.[46]
Dosage and Instructions
The label states to take 5 capsules daily, with or without food. If you do AM/PM dosing, you could consider splitting the dose to keep the active ingredients in your plasma more often, but it's not necessary to do that.
Conclusion: CORE Prostate rounds out the Lifeline Series Launch
Core Nutritionals Prostate has a ton of well-researched and efficacious ingredients for prostate health. One of the things we love about it is it doesn't contain anything that would be overdosed if you were to stack it with, say, a multivitamin. Another possibility is stacking it with a high-quality omega-3 supplement – which has also been shown to be beneficial for prostate health.[47]
On top of the diet that avoids insulin resistance[4] (stop using seed oils and abusing refined sugar!), prostate issues have been associated with chronic systemic inflammation in the research literature,[48] so we recommend considering a good anti-inflammatory supplement as well. To learn more about Core SOOTHE, which also launched in the Lifeline Series, read our article titled Core SOOTHE: Comprehensive Anti-Inflammatory Supplement.
Now that's a stack for a Lifeline.
Core Nutritionals PROSTATE – Deals and Price Drop Alerts
Get Price Alerts
No spam, no scams.
Disclosure: PricePlow relies on pricing from stores with which we have a business relationship. We work hard to keep pricing current, but you may find a better offer.
Posts are sponsored in part by the retailers and/or brands listed on this page.












Comments and Discussion (Powered by the PricePlow Forum)