If you've been in the alternative health sphere for a while you've no doubt heard of glutathione (GSH), which we call the body's master antioxidant.
We say GSH is the master antioxidant because it's the most abundant[1] and one of the most powerful[2] antioxidants in the human body. But the best thing about the compound is that your body produces its own glutathione,[1] as part of its natural antioxidant defense systems.
It appears that GSH levels are a crucial factor in overall health. Controlled longevity studies are extremely difficult to do in humans, but research on simpler organisms speaks for itself. For example, studies on Saccharomyces cerevisiae, also known as brewer's yeast, consistently show that organisms with higher GSH levels live significantly longer than those with less GSH.

Revive MD is out with a standalone NAC product. The much-discussed glutathione precursor has a wide-ranging array of benefits, from supporting liver function to psychological support.
In humans, GSH depletion has been associated with the onset of serious diseases ranging from dementia[3,4] to diabetes, and obesity.[5,6]
The Problem: Oral Glutathione Doesn't Work Very Well
The problem is that directly supplementing with glutathione has proven to be quite a challenge. Studies have found the bioavailability of oral GSH supplements is bad enough that it's not possible to raise GSH blood levels by swallowing pure GSH.[7]
What about special GSH supplements?
Over the years, special GSH preparations and compounds have been developed by manufacturers who claim that their process increases the oral bioavailability of the antioxidant.
While we do think that some of these GSH preparations would probably work well for most people, the high cost is a big issue.
The Solution: GSH Precursor Supplementation (NAC)
Poor bioavailability of target molecules is a common problem in supplement science. The best way of getting around it is usually to take the precursors to that molecule instead. Oftentimes, they're much more bioavailable than the target itself.
Fortunately, this is definitely a workable solution in the case of GSH. Research consistently shows that supplementation with GSH precursors, like cysteine and glycine, can go a long way toward restoring normal levels in people whose GSH has been depleted.[6,8]
As we'll see when we get into the research, N-acetylcysteine (NAC) is one of the best supplements you can take if your goal is to boost GSH production.
The best part is that it's much less expensive than designer GSH supplements – usually half the price or less based on our current market research.
Let's do a deep dive into how NAC can benefit your health, but first, check the PricePlow news and deals:
Revive MD NAC – Deals and Price Drop Alerts
Get Price Alerts
No spam, no scams.
Disclosure: PricePlow relies on pricing from stores with which we have a business relationship. We work hard to keep pricing current, but you may find a better offer.
Posts are sponsored in part by the retailers and/or brands listed on this page.
N-acetylcysteine Research
Once you understand the role of GSH in your body, it's easy to see that your health depends immensely on keeping GSH production at appropriate levels. Again, it's the most powerful and ubiquitous antioxidant in the body, which means it's used for pretty much every metabolic process.
Out of control oxidative stress has been linked to rapid aging and the onset of major disease, including cancer, cardiovascular disease, respiratory disease, rheumatoid arthritis, kidney disease, and sexual dysfunction.[9]
There's a bidirectional relationship between oxidative stress and inflammation. Oxidative stress makes inflammation worse, and inflammation makes oxidative stress worse.[10,11]
And given that chronic systemic inflammation damages basically every tissue in the body, the potentially catastrophic results of GSH depletion are scarily apparent.
This is also, of course, a key mechanism underlying the link between GSH depletion and the metabolic and neurological diseases that we discussed in the introduction.
So if you read the following research thinking that NAC is simply too good to be true, remember that we're dealing with a very fundamental mechanism for human health and performance – the management of oxidative stress and inflammation. This goes a long way toward explaining NAC's extraordinary potential to improve human health.[12]
-
The big one: NAC improves liver function and detoxification
Let's start with the reason most people seem to get interested in supplementing with NAC – its effect on liver health.
More specifically, there's been a huge surge of NAC-related interest in recent years thanks to the popularization of the fact that NAC can help your body manage the toxicity of alcohol. College students all over the U.S. swear by NAC's ability to promote recovery from a night of drinking, while preventing or diminishing the intensity of hangovers.
This claim is based on animal studies showing that NAC can reduce oxidative stress[13,14] and thus protects against some of alcohol's damaging effect.[15]
In one study, rats given NAC and alcohol had lower liver enzymes than rats given alcohol alone.[15] Lower liver enzymes is a good thing, because damaged or inflamed liver cells tend to leak their contents into the blood, including these enzymes.[16] So, lower liver enzyme levels imply less damage and inflammation to liver tissue.
In one especially interesting study, researchers took a population of rats who demonstrated a preference for drinking alcohol – alcoholic rats, basically – and gave them an NAC supplement. Compared to rats who didn't get NAC, the NAC-treated rats spontaneously drank 65% less alcohol when given access to as much alcohol as they wanted.[17]
Because of this effect, some researchers actually propose NAC should be used for the treatment or management of alcohol use disorder in humans.[18]
So how exactly does NAC protect your liver from toxic insults? You guessed it – by restoring glutathione levels in liver cells.[19]
In fact, NAC is so good at protecting the liver from toxins that it's actually a first-line treatment for acetaminophen toxicity.[20]
Please note: NAC probably will not completely prevent liver toxicity induced by alcohol consumption. For example, one rat study where liver enzymes were measured, the rats who got NAC and alcohol still had higher liver enzymes than those who got neither.[21]
In other words, taking NAC is not a license to drink as much as you want. The evidence suggests that it can significantly reduce, but not completely prevent, alcohol-induced liver injury.
In one study, treatment with NAC reduced liver enzymes by about 36% in rats who consumed alcohol – but even the alcohol rats who got NAC had 37% higher liver enzymes than those who only got NAC.[21] EtOH is an abbreviation for ethanol.
So how effective is it? Well, in the study we just mentioned, rats who got NAC and alcohol had an alanine transaminase (ALT) level of about 172, compared to about 267 in those who only got alcohol, and 126 in rats who got NAC without alcohol. So even if you take NAC when drinking, this study predicts that you'll still experience a significant increase in liver enzyme blood levels.
Can NAC combat hangovers? Its effect on aldehyde dehydrogenase (ALDH) enzymes
Part of NAC's ability to fortify the body against the ravages of heavy drinking can be attributed to its effect on aldehyde dehydrogenase (ALDH), the enzyme responsible for detoxifying the aldehydes produced when the body metabolizes alcohol.[22] These aldehyde metabolites are extremely toxic – the sooner you can eliminate them, the better.
Well, the good news is that NAC has been shown in at least one animal study to significantly upregulate ALDH activity.[23]
There's definitely not a ton of research on this subject, so it's hard to draw definitive conclusions about it right now. But given NAC's positive effect on overall liver health and function, it wouldn't surprise us in the least to see significant upregulation of ALDH and ADH (alcohol dehydrogenase, the enzyme that converts alcohol into aldehydes).
-
The psychological and neurological benefits of NAC
Because of its ability to boost GSH production, NAC can have some significant neuroprotective effects.
For one thing, it helps balance glutamate activity in the brain through its provision of cysteine, which helps trigger negative feedback on the amount of free glutamate released by neurons.[24]
Excessive glutamate activity can cause uncontrolled neuron firing, a condition called excitotoxicity that is essentially a form of low-grade neuroinflammation.[25] Because of its ability to damage brain tissue and impair cognitive function, glutamate-induced excitotoxicity has been proposed as a factor in the onset of serious psychiatric disorders.[26]
According to a meta-analysis and randomized, double-blind, placebo-controlled study on the subject, NAC has been shown to improve symptoms of OCD.[27,28]
An animal study demonstrated that NAC treatment can reverse some of the neurological changes associated with schizophrenia.[29]
As it turns out, NAC's ability to spontaneously decrease alcohol use may apply to other drugs as well. One study in men and women age 18 to 21 found that four weeks of NAC supplementation decreased the subjects' number of daily marijuana use, from 15.9 "hits" at the beginning of the study, to 11.9 by week four.[30] That's about a 25% reduction in marijuana use, just from supplementing NAC.
So, summing all this up, what is the underlying theme? NAC seems to help stabilize brain function through GSH upregulation. This makes it potentially useful in a wide range of neurological ailments that have traditionally been seen as intractable – as one 2013 editorial advocating for more NAC research takes pains to point out.[31]
-
The respiratory benefits of NAC
Yet another bodily system affected by GSH production is the respiratory system. Depletion of GSH is associated with the onset of respiratory illnesses like chronic obstructive pulmonary disease (COPD),[32] idiopathic pulmonary fibrosis,[33] and cystic fibrosis.[34]
It's no surprise, then, that a 2016 meta-analysis of NAC literature concludes that the compound has been shown to significantly improve symptoms of COPD.[35]
A similar review from the year 2000 found that NAC can improve symptoms of bronchitis as well,[36] partly because its upregulation of GSH can actually thin the mucus produced in your airways.
And of course, NAC has proven its weight in gold the past few years, combating more "modern" respiratory illnesses with incredible results.[37,38]
-
NAC's pro-fertility effect
Most of us have probably heard by now that oxidative stress can also wreak havoc on fertility – in both men and women.
One particularly interesting study looking at NAC's effects on this was conducted in men with varicocele.
Varicocele is a condition in which veins exiting the testes become varicose, leading to the reflux of blood and the accumulation of toxins in testicular tissue. In some cases, varicocele can negatively affect fertility and testosterone production.[39,40]
Men enrolled in the study first had surgical correction of their varicocele, and then were randomized to either an NAC group or a placebo group so the researchers could track the impact of each treatment on their fertility.
By the end of the three month study period, the men taking 600 milligrams of NAC daily showed significantly better sperm quality than the men who took the placebo control.[41]
In another study, men with varicocele were randomized to one of four groups: a 600 milligram NAC per day group, a group given 200 micrograms of selenium per day, a placebo group, and finally, a group that got both the 600 milligrams of NAC and 200 micrograms of selenium.
Although the combination NAC and selenium group showed the most improvement in sperm quality by the end of the treatment period, the group that got only 600 milligrams of NAC also improved substantially.[42]
There's also evidence that NAC can improve fertility in women with polycystic ovary syndrome (PCOS) by improving the severity of their symptoms.[43]
-
The anti-diabetic effects of NAC
Inflammation and oxidative stress can play a huge role in the onset of insulin resistance, the metabolic syndrome, and type 2 diabetes (T2D) as well.[44] As we alluded to in the introduction, GSH depletion is a feature of metabolic dysfunction, and is consistently observed in patients with full blown T2D.[5,6]
Although NAC seems to not improve symptoms in people with existing T2D,[45] animal studies suggest it can help prevent the onset of diabetes by normalizing blood sugar and reducing inflammation.[46,47]
-
NAC's cardioprotective effects
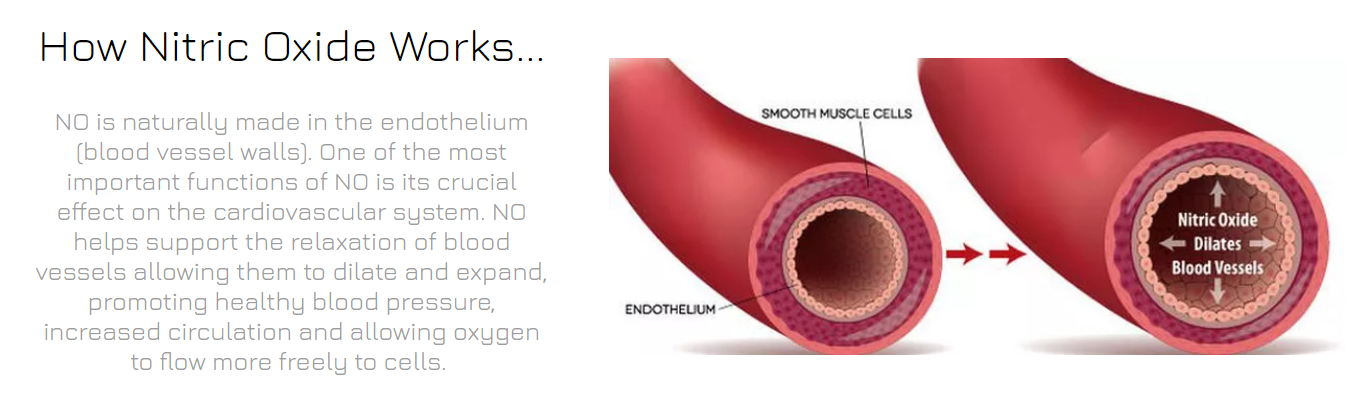
NAC has also been shown to increase the body's production of nitric oxide (NO), a gaseous molecule produced by arterial cells that causes vasodilation, an expansion of blood vessels that leads to improved circulation and causes blood pressure and resting heart rate to drop.[48]
Since reduced NO activity is a feature of cardiovascular disease (CVD),[49] this can potentially help prevent or improve the symptoms of CVD.
-
NAC can boost immunity
Finally, NAC has been shown to help improve the function of the human immune system, and has been extraordinarily useful the past few years.[37,38] According to one study, NAC can "fine tune" immune responses independently of its antioxidant effects.[50] According to the authors of this study, the GSH created by NAC supplementation doesn't just fight oxidative stress, but also it plays an important signaling role for the immune system.
It might have something to do with the fact that sulfur, a molecule that's abundant in NAC, modulates immune function via the H2S signaling pathway.[51]
Conclusion

Of course, when the rubber meets the road, there are limitations, as we saw in the study where NAC was found to be ineffective for improving symptoms of full blown type 2 diabetes.
But if you have a stubborn problem and aren't sure what to do about it, it's worth bringing up NAC with your doctor to see what they think about starting you on an NAC supplement.
Revive MD NAC – Deals and Price Drop Alerts
Get Price Alerts
No spam, no scams.
Disclosure: PricePlow relies on pricing from stores with which we have a business relationship. We work hard to keep pricing current, but you may find a better offer.
Posts are sponsored in part by the retailers and/or brands listed on this page.






Comments and Discussion (Powered by the PricePlow Forum)