Zinc is an essential mineral that has a multitude of biological roles in the body. In the ongoing "immunity crisis" that began in 2020, zinc supplementation gained steam, as it's well-known that supplementation of various forms of the mineral (especially at high enough doses) reduces symptoms of the common cold.[1-11]
Zinc: the hottest mineral in 2020
With those results, it's no surprise that nearly every company put out either a zinc supplement or a zinc-based immunity supplement in the past year - likely both. This proved fruitful, since there was a very strong correlation between healthy zinc status and successful recovery from the novel virus at hand,[12-14] a solid improvement when used in early treatment (often alongside other antiviral drugs),[15,16] and even a fair amount of success when used in late treatment.[17,18]

Revive MD's Zinc is out, and it brings 50mg elemental zinc from OptiZinc (zinc monomethionine). They explain the decision lower down.
The questions for a supplement brand's formulator come down to what type of zinc to use and at what dose.
Revive MD Zinc: 50mg Zinc from OptiZinc zinc monomethionine
Revive MD is a supplement brand founded by Dr. Domenic Iacovone and Matt Jansen, and it's become well-known for their upheaval of the health segments in the sports nutrition industry. The team has brought standards up in the industry thanks to their incredible formulas status as a third-party lab-tested brand that is safe for drug-tested athletes to use.
Revive MD already has an Immune Multi, but many of their users wanted higher-dosed zinc that's also third-party tested and trusted. In response, the team chose an extremely high bioavailability zinc ingredient - OptiZinc - and put enough in to yield 50mg zinc in their new Revive MD Zinc supplement.
In this article, we get into some other benefits to zinc supplementation (it's not just about immunity!) and discuss the differences and specific research on OptiZinc. Before that, you can compare our coupon-powered prices on Revive MD Zinc and sign up for our alerts:
Revive MD Zinc – Deals and Price Drop Alerts
Get Price Alerts
No spam, no scams.
Disclosure: PricePlow relies on pricing from stores with which we have a business relationship. We work hard to keep pricing current, but you may find a better offer.
Posts are sponsored in part by the retailers and/or brands listed on this page.
This area is reserved for Team PricePlow's upcoming Ingredients video.
Subscribe to our channel and sign up for notifications so you catch it when it goes live!
What is zinc? It's not just about immunity
Zinc is an essential dietary mineral that plays a significant role in our body's chemistry. It's often used as a catalyst for other reactions. In fact, it is the second-most abundant trace mineral within the body.[19]
Highly bioavailable zinc is most commonly found in meat and eggs, with oysters being a very good source of the mineral. The issue is, diets have trended away from meat and eggs, and oysters aren't exactly household foods these days. Plant-based diets are on the rise, and legumes technically have a good amount of zinc, but they're not always first on the menu. On the plant-based front, certain legumes also have high zinc content, but it's generally of lower bioavailability because legumes (and grains) contain phytates that inhibit zinc's absorption.[20,21]
This trend may be leading to a low level of zinc deficiency, which must be supplemented around. But not all zinc supplements are the same, and it's best to use a high bioavailability zinc.
Issues with zinc deficiency
Severe zinc deficiency is less common in Western countries, but could lead to hair loss, diarrhea, impotence, hypogonadism in males, and eye and skin lesions.[22-25] More commonly with lower levels of deficiency, we see impaired immune function,[26] poor growth, infertility, lower testosterone levels, odd taste, and overall lethargic / low energy levels.[25,27-29] that could lead to weight loss and further deficiency.
Benefits of Zinc supplementation: Immunity and beyond
In the introduction, we already touched upon zinc's usefulness against cold viruses,[1-18] especially when paired with a zinc ionophore, a combination that can impair the replication of various RNA viruses, including poliovirus and influenza.[30]
But first, some additional immune benefits
Zinc has a critical role in the proper functioning of important immune cells such as natural killer (NK) cells, neutrophils, and macrophages.[26] Each of these are key components of the innate immune system, which identifies cells that have been infected and destroy them through apoptosis (cell death) or phagocytosis. This is done to ensure infected cells cannot harm other cells.
Inversely, when zinc deficient, the body cannot proliferate T-cells and B-cells.[26] These are involved in the adaptive immune system, which helps the body build immunity via antibody creation. Finally, zinc is an antioxidant that can support cell membranes and protect them from damage caused by free radicals.[26]
Revive MD's athletes need the best
However, most of Revive MD's customers are generally healthy athletes looking to be their best, so we're going to slant the rest of the article towards some of the benefits that may lead to better performance, and then get into OptiZinc itself.
Given zinc's abundance throughout our systems, the benefits of supplementation (i.e. the benefits of not being deficient) span several health systems. Below is a list of research where the effects are consistent:
-
Improved Mood
Several studies have shown zinc to be effective in terms of mood states in both men and women.[31-35] The studies generally last a few months and almost universally have positive outcomes. One study determined a quality reduction in anxiety, as well.[35]
-
Increased Testosterone
Revive MD comes out swinging in 2021! Listen to co-founder Dr. Domenic Iacovone on Episode #042
Both sedentary individuals and athletes who train to fatigue often see testosterone levels improve with zinc supplementation.[36-39] Free testosterone improved in a couple of these studies as well,[36,39] and this is important since free testosterone is unbound and readily available.
-
Improved Blood Glucose Levels and Insulin Sensitivity
We generally see a reduction in blood glucose[40-42] and improved insulin sensitivity,[41,42] especially when given to obese individuals who were likely to be deficient. The studies are generally carried out in adolescents, who tend to lose weight once their zinc deficiencies are corrected.
Satisfying a satiety signal with other essential nutrients
There is a strong connection between hunger and satiety signals and essential minerals (such as zinc), amino acids, and fatty acids found in nutrient-dense foods like red meat and seafood. When appropriate foods are not provided to children, hunger runs rampant, as the body is requesting nutrition, not just unsatisfactory empty "calories".
-
Reduction of Acne
Several studies have shown high doses of zinc may lead to lower acne,[43-45] but lower doses (30mg elemental zinc) have shown success as well.[46]
-
Improved Health Markers (IGF-1 up, Insulin down, CRP down, antioxidant status up, T3 and T4)
On the note of blood levels, Revive MD is now offering free blood tests!
A myriad of general health markers seem to improve with zinc supplementation. These range from IGF-1[47-49] to fasting insulin[41,42,50,51] to C-Reactive Protein (CRP)[41,50,52-54] to antioxidant levels[54,55] to thyroid hormones.[36,39]
-
Improved Cognition
Zinc studies have yielded cognitive improvements in both young and old.[56,57]
-
Improved general well-being
Unsurprising given the above research, studies that measure "subjective well-being" or similar metrics have yielded moderate success.[31,58] The body simply works better when zinc is not deficient.
This isn't necessarily stating that every person taking zinc is going to be happier with better testosterone and T4 levels. Rather, it's better to say that we often see improvements in the above metrics when correcting deficiency.
Why OptiZinc?

L-OptiZinc is a patented form of zinc from Lonza. It can come as zinc monomethionine or as zinc monomethionine blended with zinc sulfate
The studies above overwhelmingly demonstrate that supplemental zinc is paramount in the face of deficiency. But why did Revive MD choose OptiZinc zinc monomethionine, especially when their Immune Multi uses a different form of zinc known as zinc bisglycinate?
Amino acid bound is best
It turns out that both versions use similar technologies - OptiZinc zinc monomethionine is a chelated form of zinc that is bound to the essential amino acid, methionine. Alternatively, the zinc bisglycinate in their Immune Multi has zinc bound to the amino acid glycine.
Both work similarly, in that they are amino acid complexes. The reasoning (which is backed by data) is that our small intestines are not that great at absorbing straight minerals. They are, however, excellent at absorbing amino acids. So what these companies have done is to bind targeted minerals (in this case, zinc) to amino acids in order to "Trojan Horse" them into the system. The body works to absorb the methionine (or glycine), and the zinc comes along for the ride, entering the bloodstream.
Differentiating the different OptiZinc forms and their patents
Made by Lonza, OptiZinc is covered by a few patents,[59-61] but it's important to note that those patents cover zinc monomethionine complexes (often blended with zinc sulfate), while Revive MD chose to go with a pure zinc monomethionine form.
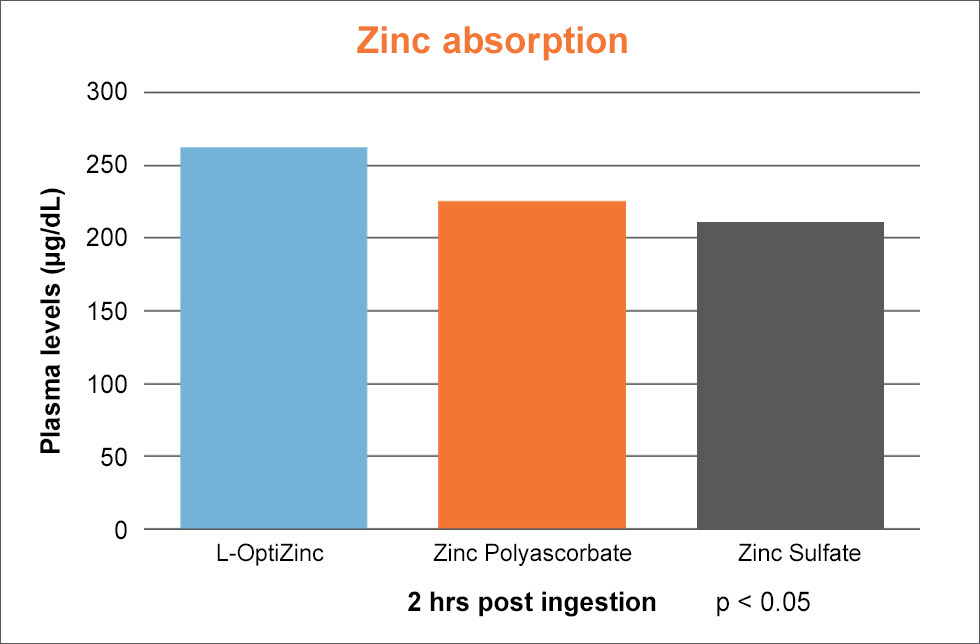
The formula provides ~21% elemental zinc from L-OptiZinc in a 1:1 complex of zinc and methionine, and Lonza claims 24% better absorption than zinc oxide with 21% better retention. They also have data showing higher plasma zinc levels than zinc polyascorbate and zinc sulfate,[62,63] and far greater bioavailability than zinc sulfate and zinc oxide,[64] Lonza also often cites improved antioxidant properties compared to zinc sulfate, zinc gluconate, zinc picolinate.[65]
Just say no to zinc oxide
Back to the OptiZinc vs. zinc bisglycinate debate, both are vastly superior to other forms of zinc on the market -- especially zinc oxide, which has awfully low bioavailability[66-68] (and in some humans, no absorption)[66] and should thus be shunned from the market.
Revive MD on the OptiZinc choice
The question is, why OptiZinc over bisglycinate? We bring in the ringer, Revive MD's Chief Compliance & Formulations Officer, William Wallace, to answer that question, since both are great forms:
"To our knowledge, there is no pharmacokinetic data available comparing equivalent doses of zinc monomethionine (OptiZinc) or zinc bisglycinate chelate in the same model. However, when cross-referencing human and animal data, we can conclude that these two likely have similar bioavailability and AUC over a 4 hour period after a single administration.
Welcome William Wallace to Revive MD, their new Chief Compliance & Formulations Officer. It's a great day when he graces our blog with a blockquote.
Further, zinc monomethionine has more data suggesting that its antioxidant properties (i.e. ability to reduce superoxide anion and hydroxyl radical accumulation in cell models) are superior to other zinc supplements (gluconate, picolinate, sulfate, oxide, and citrate). Currently, we are not aware of data showing similar antioxidant potential of zinc bisglycinate chelate. Although we are not claiming that this property is not matched in the TRAACs version, we thought that the more robust history of research with the monomethionine version gave this one a slight edge when it came to an affordable standalone zinc product."
-- William Wallace, Revive MD Chief Compliance & Formulations Officer
Dosage
It's worth a reminder that Revive MD Zinc provides 50mg elemental zinc -- not 50mg OptiZinc. It's critical to note this on labels to avoid over- or under-dosing your supplements. Since zinc monomethionine is roughly 21% zinc by weight, we need 238mg zinc monomethionine / OptiZinc to get our 50mg dose.
Read labels carefully, because all zinc supplements are bound differently, and we're generally looking to supplement 30-50mg zinc per day. Revive MD, being a brand for hard-charging athletes, is on the higher end of that scale.
Revive MD keeps you going
On top of their status as a BSCG-certified company for drug-tested athletes, we love the way Revive MD formulates and provides reasoning for their formulations.
In a perfect world, we wouldn't have to concern ourselves with finding quality zinc supplements. Mineral-dense food such as red meat, eggs, and shellfish should be able to take care of it. But we live in a world with nutrient-scarce processed foods, novel cold viruses, cheap zinc oxide supplements, and non-stop fear mongering without mention of metabolic health and appropriate eating.

Supplements formulated to optimize your health! See them all on our Revive MD page on PricePlow.
In the state of today's society, it's great that we can count on companies like Revive MD to provide us with the tools to live in it as well as possible. When it comes to immunity and virility, one of the first things we check is one's zinc status, and Revive MD has us convinced that OptiZinc needs to be in the conversation more often.
Revive MD Zinc – Deals and Price Drop Alerts
Get Price Alerts
No spam, no scams.
Disclosure: PricePlow relies on pricing from stores with which we have a business relationship. We work hard to keep pricing current, but you may find a better offer.
Posts are sponsored in part by the retailers and/or brands listed on this page.








Comments and Discussion (Powered by the PricePlow Forum)